We use essential cookies to make Venngage work. By clicking “Accept All Cookies”, you agree to the storing of cookies on your device to enhance site navigation, analyze site usage, and assist in our marketing efforts.
Manage Cookies
Cookies and similar technologies collect certain information about how you’re using our website. Some of them are essential, and without them you wouldn’t be able to use Venngage. But others are optional, and you get to choose whether we use them or not.
Strictly Necessary Cookies
These cookies are always on, as they’re essential for making Venngage work, and making it safe. Without these cookies, services you’ve asked for can’t be provided.
Show cookie providers
- Google Login
Functionality Cookies
These cookies help us provide enhanced functionality and personalisation, and remember your settings. They may be set by us or by third party providers.
Performance Cookies
These cookies help us analyze how many people are using Venngage, where they come from and how they're using it. If you opt out of these cookies, we can’t get feedback to make Venngage better for you and all our users.
- Google Analytics
Targeting Cookies
These cookies are set by our advertising partners to track your activity and show you relevant Venngage ads on other sites as you browse the internet.
- Google Tag Manager
- Infographics
- Daily Infographics
- Graphic Design
- Graphs and Charts
- Data Visualization
- Human Resources
- Training and Development
- Beginner Guides
Blog Case Study

How to Present a Case Study like a Pro (With Examples)
By Danesh Ramuthi , Sep 07, 2023

Okay, let’s get real: case studies can be kinda snooze-worthy. But guess what? They don’t have to be!
In this article, I will cover every element that transforms a mere report into a compelling case study, from selecting the right metrics to using persuasive narrative techniques.
And if you’re feeling a little lost, don’t worry! There are cool tools like Venngage’s Case Study Creator to help you whip up something awesome, even if you’re short on time. Plus, the pre-designed case study templates are like instant polish because let’s be honest, everyone loves a shortcut.
Click to jump ahead:
What is a case study presentation?
What is the purpose of presenting a case study, how to structure a case study presentation, how long should a case study presentation be, 5 case study presentation examples with templates, 6 tips for delivering an effective case study presentation, 5 common mistakes to avoid in a case study presentation, how to present a case study faqs.
A case study presentation involves a comprehensive examination of a specific subject, which could range from an individual, group, location, event, organization or phenomenon.
They’re like puzzles you get to solve with the audience, all while making you think outside the box.
Unlike a basic report or whitepaper, the purpose of a case study presentation is to stimulate critical thinking among the viewers.
The primary objective of a case study is to provide an extensive and profound comprehension of the chosen topic. You don’t just throw numbers at your audience. You use examples and real-life cases to make you think and see things from different angles.

The primary purpose of presenting a case study is to offer a comprehensive, evidence-based argument that informs, persuades and engages your audience.
Here’s the juicy part: presenting that case study can be your secret weapon. Whether you’re pitching a groundbreaking idea to a room full of suits or trying to impress your professor with your A-game, a well-crafted case study can be the magic dust that sprinkles brilliance over your words.
Think of it like digging into a puzzle you can’t quite crack . A case study lets you explore every piece, turn it over and see how it fits together. This close-up look helps you understand the whole picture, not just a blurry snapshot.
It’s also your chance to showcase how you analyze things, step by step, until you reach a conclusion. It’s all about being open and honest about how you got there.
Besides, presenting a case study gives you an opportunity to connect data and real-world scenarios in a compelling narrative. It helps to make your argument more relatable and accessible, increasing its impact on your audience.
One of the contexts where case studies can be very helpful is during the job interview. In some job interviews, you as candidates may be asked to present a case study as part of the selection process.
Having a case study presentation prepared allows the candidate to demonstrate their ability to understand complex issues, formulate strategies and communicate their ideas effectively.
The way you present a case study can make all the difference in how it’s received. A well-structured presentation not only holds the attention of your audience but also ensures that your key points are communicated clearly and effectively.
In this section, let’s go through the key steps that’ll help you structure your case study presentation for maximum impact.
Let’s get into it.
Open with an introductory overview
Start by introducing the subject of your case study and its relevance. Explain why this case study is important and who would benefit from the insights gained. This is your opportunity to grab your audience’s attention.

Explain the problem in question
Dive into the problem or challenge that the case study focuses on. Provide enough background information for the audience to understand the issue. If possible, quantify the problem using data or metrics to show the magnitude or severity.

Detail the solutions to solve the problem
After outlining the problem, describe the steps taken to find a solution. This could include the methodology, any experiments or tests performed and the options that were considered. Make sure to elaborate on why the final solution was chosen over the others.

Key stakeholders Involved
Talk about the individuals, groups or organizations that were directly impacted by or involved in the problem and its solution.
Stakeholders may experience a range of outcomes—some may benefit, while others could face setbacks.
For example, in a business transformation case study, employees could face job relocations or changes in work culture, while shareholders might be looking at potential gains or losses.
Discuss the key results & outcomes
Discuss the results of implementing the solution. Use data and metrics to back up your statements. Did the solution meet its objectives? What impact did it have on the stakeholders? Be honest about any setbacks or areas for improvement as well.
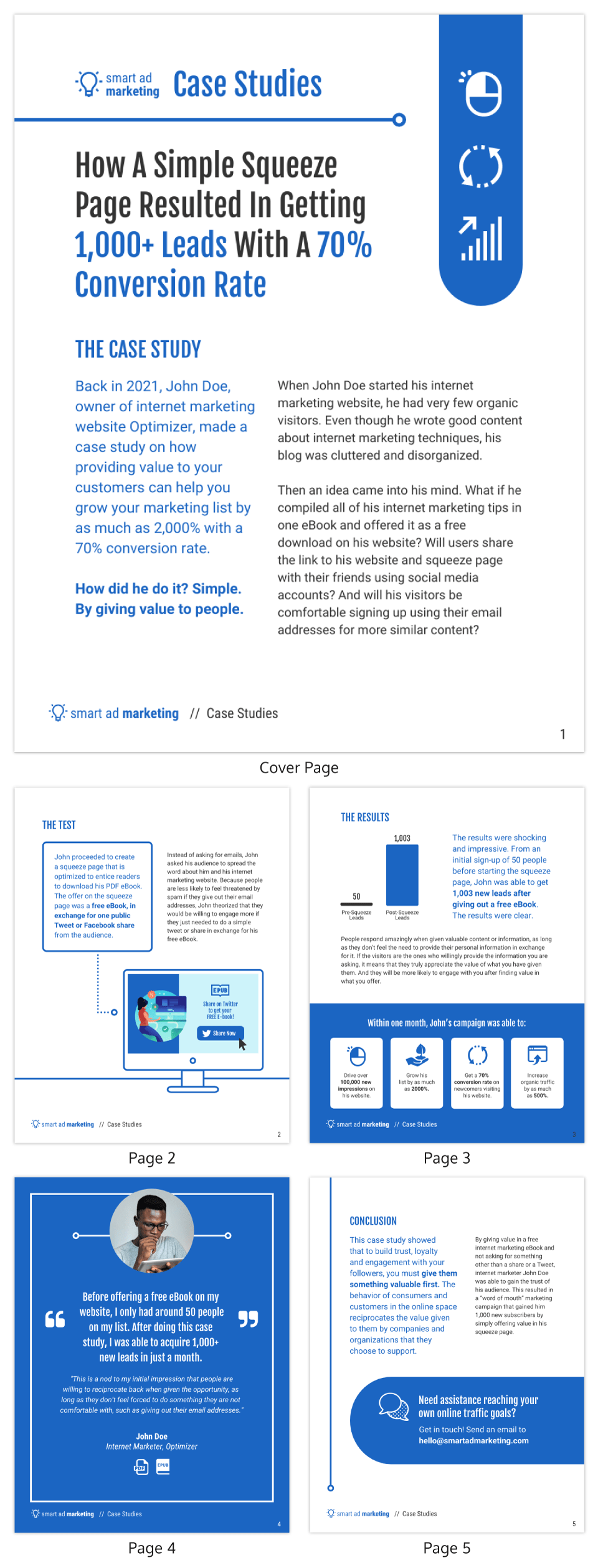
Include visuals to support your analysis
Visual aids can be incredibly effective in helping your audience grasp complex issues. Utilize charts, graphs, images or video clips to supplement your points. Make sure to explain each visual and how it contributes to your overall argument.
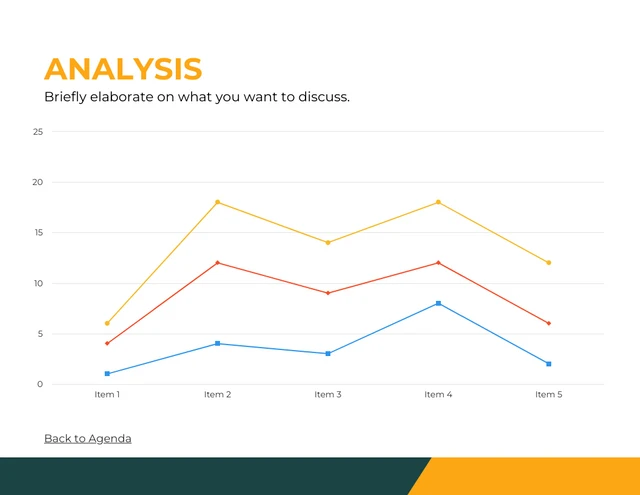
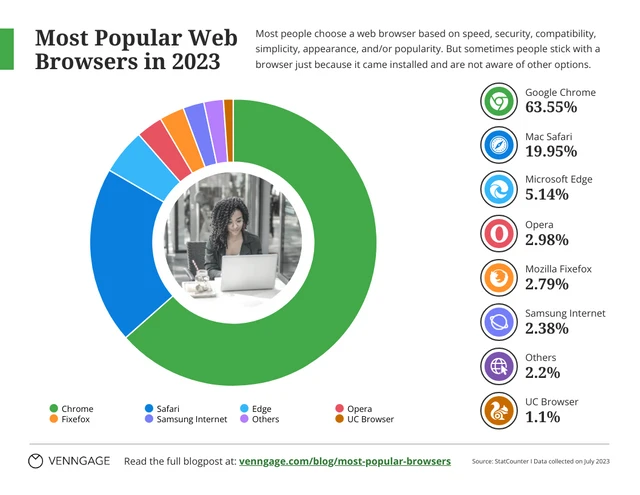
Pie charts illustrate the proportion of different components within a whole, useful for visualizing market share, budget allocation or user demographics.
This is particularly useful especially if you’re displaying survey results in your case study presentation.
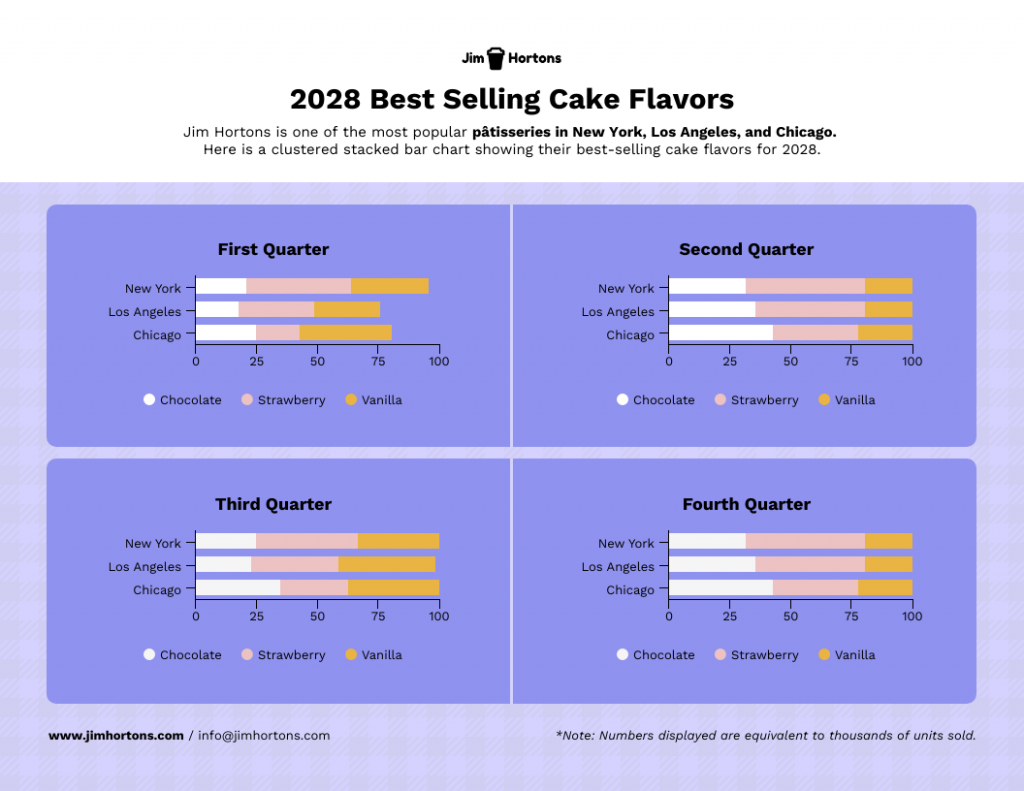
Stacked charts on the other hand are perfect for visualizing composition and trends. This is great for analyzing things like customer demographics, product breakdowns or budget allocation in your case study.
Consider this example of a stacked bar chart template. It provides a straightforward summary of the top-selling cake flavors across various locations, offering a quick and comprehensive view of the data.
Not the chart you’re looking for? Browse Venngage’s gallery of chart templates to find the perfect one that’ll captivate your audience and level up your data storytelling.
Recommendations and next steps
Wrap up by providing recommendations based on the case study findings. Outline the next steps that stakeholders should take to either expand on the success of the project or address any remaining challenges.
Acknowledgments and references
Thank the people who contributed to the case study and helped in the problem-solving process. Cite any external resources, reports or data sets that contributed to your analysis.
Feedback & Q&A session
Open the floor for questions and feedback from your audience. This allows for further discussion and can provide additional insights that may not have been considered previously.
Closing remarks
Conclude the presentation by summarizing the key points and emphasizing the takeaways. Thank your audience for their time and participation and express your willingness to engage in further discussions or collaborations on the subject.

Well, the length of a case study presentation can vary depending on the complexity of the topic and the needs of your audience. However, a typical business or academic presentation often lasts between 15 to 30 minutes.
This time frame usually allows for a thorough explanation of the case while maintaining audience engagement. However, always consider leaving a few minutes at the end for a Q&A session to address any questions or clarify points made during the presentation.
When it comes to presenting a compelling case study, having a well-structured template can be a game-changer.
It helps you organize your thoughts, data and findings in a coherent and visually pleasing manner.
Not all case studies are created equal and different scenarios require distinct approaches for maximum impact.
To save you time and effort, I have curated a list of 5 versatile case study presentation templates, each designed for specific needs and audiences.
Here are some best case study presentation examples that showcase effective strategies for engaging your audience and conveying complex information clearly.
1 . Lab report case study template
Ever feel like your research gets lost in a world of endless numbers and jargon? Lab case studies are your way out!
Think of it as building a bridge between your cool experiment and everyone else. It’s more than just reporting results – it’s explaining the “why” and “how” in a way that grabs attention and makes sense.
This lap report template acts as a blueprint for your report, guiding you through each essential section (introduction, methods, results, etc.) in a logical order.

Want to present your research like a pro? Browse our research presentation template gallery for creative inspiration!
2. Product case study template
It’s time you ditch those boring slideshows and bullet points because I’ve got a better way to win over clients: product case study templates.
Instead of just listing features and benefits, you get to create a clear and concise story that shows potential clients exactly what your product can do for them. It’s like painting a picture they can easily visualize, helping them understand the value your product brings to the table.
Grab the template below, fill in the details, and watch as your product’s impact comes to life!

3. Content marketing case study template
In digital marketing, showcasing your accomplishments is as vital as achieving them.
A well-crafted case study not only acts as a testament to your successes but can also serve as an instructional tool for others.
With this coral content marketing case study template—a perfect blend of vibrant design and structured documentation, you can narrate your marketing triumphs effectively.

4. Case study psychology template
Understanding how people tick is one of psychology’s biggest quests and case studies are like magnifying glasses for the mind. They offer in-depth looks at real-life behaviors, emotions and thought processes, revealing fascinating insights into what makes us human.
Writing a top-notch case study, though, can be a challenge. It requires careful organization, clear presentation and meticulous attention to detail. That’s where a good case study psychology template comes in handy.
Think of it as a helpful guide, taking care of formatting and structure while you focus on the juicy content. No more wrestling with layouts or margins – just pour your research magic into crafting a compelling narrative.
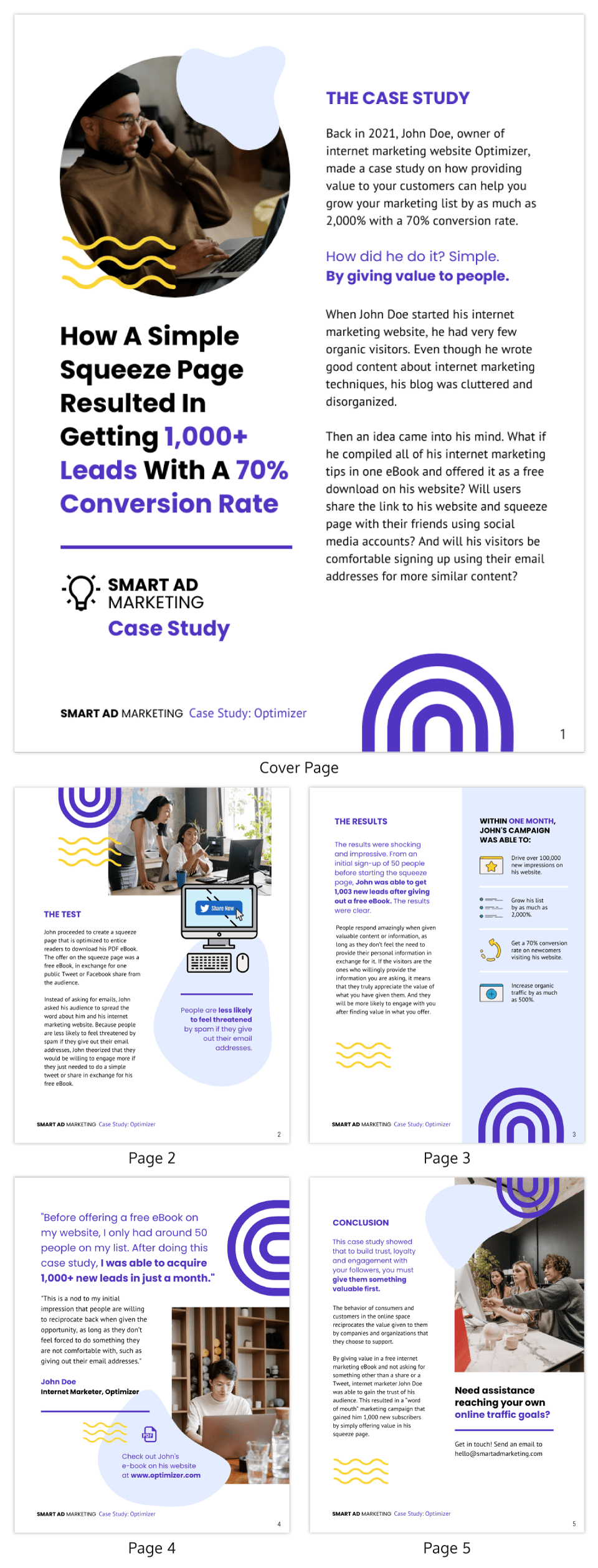
5. Lead generation case study template
Lead generation can be a real head-scratcher. But here’s a little help: a lead generation case study.
Think of it like a friendly handshake and a confident resume all rolled into one. It’s your chance to showcase your expertise, share real-world successes and offer valuable insights. Potential clients get to see your track record, understand your approach and decide if you’re the right fit.
No need to start from scratch, though. This lead generation case study template guides you step-by-step through crafting a clear, compelling narrative that highlights your wins and offers actionable tips for others. Fill in the gaps with your specific data and strategies, and voilà! You’ve got a powerful tool to attract new customers.
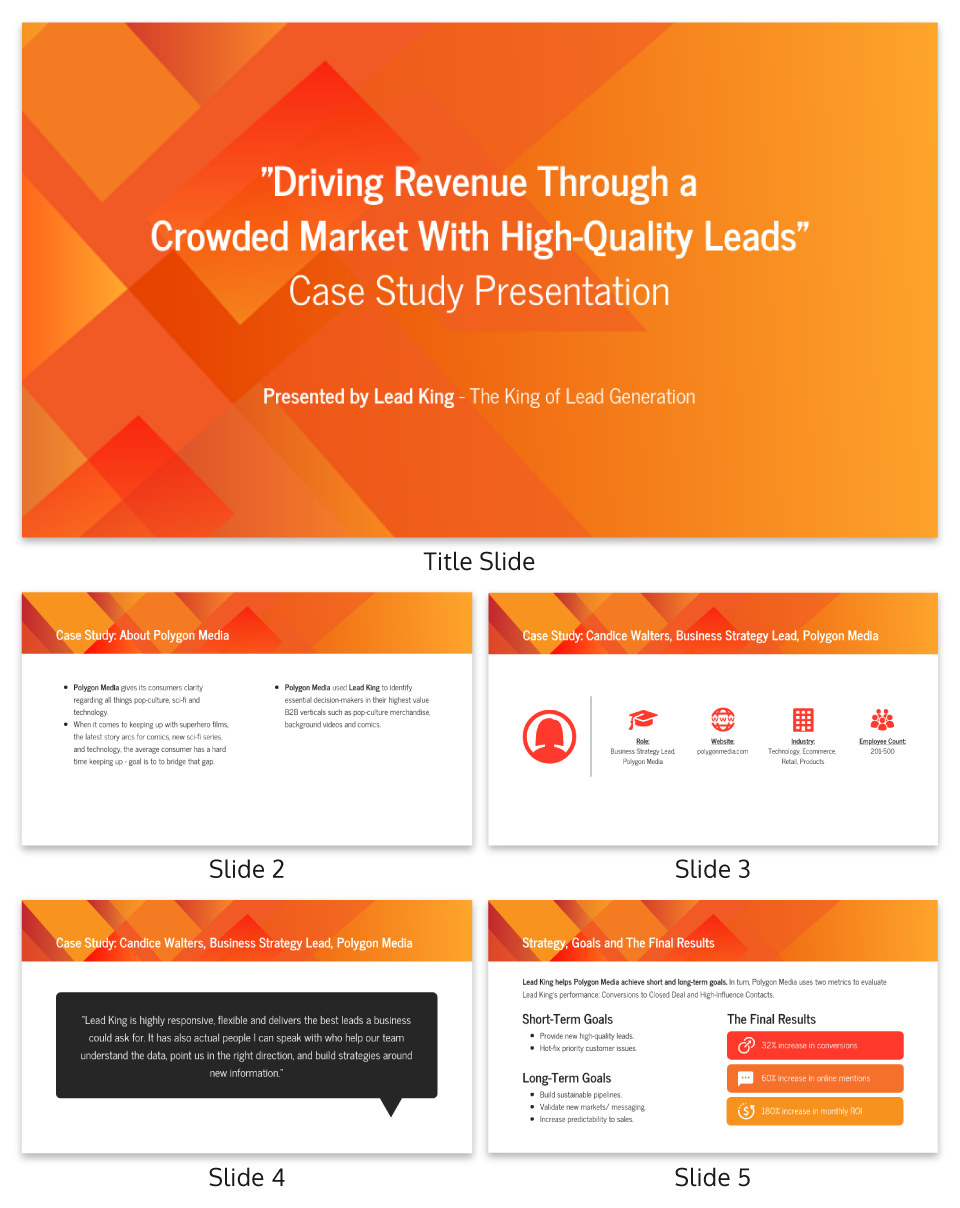
Related: 15+ Professional Case Study Examples [Design Tips + Templates]
So, you’ve spent hours crafting the perfect case study and are now tasked with presenting it. Crafting the case study is only half the battle; delivering it effectively is equally important.
Whether you’re facing a room of executives, academics or potential clients, how you present your findings can make a significant difference in how your work is received.
Forget boring reports and snooze-inducing presentations! Let’s make your case study sing. Here are some key pointers to turn information into an engaging and persuasive performance:
- Know your audience : Tailor your presentation to the knowledge level and interests of your audience. Remember to use language and examples that resonate with them.
- Rehearse : Rehearsing your case study presentation is the key to a smooth delivery and for ensuring that you stay within the allotted time. Practice helps you fine-tune your pacing, hone your speaking skills with good word pronunciations and become comfortable with the material, leading to a more confident, conversational and effective presentation.
- Start strong : Open with a compelling introduction that grabs your audience’s attention. You might want to use an interesting statistic, a provocative question or a brief story that sets the stage for your case study.
- Be clear and concise : Avoid jargon and overly complex sentences. Get to the point quickly and stay focused on your objectives.
- Use visual aids : Incorporate slides with graphics, charts or videos to supplement your verbal presentation. Make sure they are easy to read and understand.
- Tell a story : Use storytelling techniques to make the case study more engaging. A well-told narrative can help you make complex data more relatable and easier to digest.

Ditching the dry reports and slide decks? Venngage’s case study templates let you wow customers with your solutions and gain insights to improve your business plan. Pre-built templates, visual magic and customer captivation – all just a click away. Go tell your story and watch them say “wow!”
Nailed your case study, but want to make your presentation even stronger? Avoid these common mistakes to ensure your audience gets the most out of it:
Overloading with information
A case study is not an encyclopedia. Overloading your presentation with excessive data, text or jargon can make it cumbersome and difficult for the audience to digest the key points. Stick to what’s essential and impactful. Need help making your data clear and impactful? Our data presentation templates can help! Find clear and engaging visuals to showcase your findings.
Lack of structure
Jumping haphazardly between points or topics can confuse your audience. A well-structured presentation, with a logical flow from introduction to conclusion, is crucial for effective communication.
Ignoring the audience
Different audiences have different needs and levels of understanding. Failing to adapt your presentation to your audience can result in a disconnect and a less impactful presentation.
Poor visual elements
While content is king, poor design or lack of visual elements can make your case study dull or hard to follow. Make sure you use high-quality images, graphs and other visual aids to support your narrative.
Not focusing on results
A case study aims to showcase a problem and its solution, but what most people care about are the results. Failing to highlight or adequately explain the outcomes can make your presentation fall flat.
How to start a case study presentation?
Starting a case study presentation effectively involves a few key steps:
- Grab attention : Open with a hook—an intriguing statistic, a provocative question or a compelling visual—to engage your audience from the get-go.
- Set the stage : Briefly introduce the subject, context and relevance of the case study to give your audience an idea of what to expect.
- Outline objectives : Clearly state what the case study aims to achieve. Are you solving a problem, proving a point or showcasing a success?
- Agenda : Give a quick outline of the key sections or topics you’ll cover to help the audience follow along.
- Set expectations : Let your audience know what you want them to take away from the presentation, whether it’s knowledge, inspiration or a call to action.
How to present a case study on PowerPoint and on Google Slides?
Presenting a case study on PowerPoint and Google Slides involves a structured approach for clarity and impact using presentation slides :
- Title slide : Start with a title slide that includes the name of the case study, your name and any relevant institutional affiliations.
- Introduction : Follow with a slide that outlines the problem or situation your case study addresses. Include a hook to engage the audience.
- Objectives : Clearly state the goals of the case study in a dedicated slide.
- Findings : Use charts, graphs and bullet points to present your findings succinctly.
- Analysis : Discuss what the findings mean, drawing on supporting data or secondary research as necessary.
- Conclusion : Summarize key takeaways and results.
- Q&A : End with a slide inviting questions from the audience.
What’s the role of analysis in a case study presentation?
The role of analysis in a case study presentation is to interpret the data and findings, providing context and meaning to them.
It helps your audience understand the implications of the case study, connects the dots between the problem and the solution and may offer recommendations for future action.
Is it important to include real data and results in the presentation?
Yes, including real data and results in a case study presentation is crucial to show experience, credibility and impact. Authentic data lends weight to your findings and conclusions, enabling the audience to trust your analysis and take your recommendations more seriously
How do I conclude a case study presentation effectively?
To conclude a case study presentation effectively, summarize the key findings, insights and recommendations in a clear and concise manner.
End with a strong call-to-action or a thought-provoking question to leave a lasting impression on your audience.
What’s the best way to showcase data in a case study presentation ?
The best way to showcase data in a case study presentation is through visual aids like charts, graphs and infographics which make complex information easily digestible, engaging and creative.
Don’t just report results, visualize them! This template for example lets you transform your social media case study into a captivating infographic that sparks conversation.

Choose the type of visual that best represents the data you’re showing; for example, use bar charts for comparisons or pie charts for parts of a whole.
Ensure that the visuals are high-quality and clearly labeled, so the audience can quickly grasp the key points.
Keep the design consistent and simple, avoiding clutter or overly complex visuals that could distract from the message.
Choose a template that perfectly suits your case study where you can utilize different visual aids for maximum impact.
Need more inspiration on how to turn numbers into impact with the help of infographics? Our ready-to-use infographic templates take the guesswork out of creating visual impact for your case studies with just a few clicks.
Related: 10+ Case Study Infographic Templates That Convert
Congrats on mastering the art of compelling case study presentations! This guide has equipped you with all the essentials, from structure and nuances to avoiding common pitfalls. You’re ready to impress any audience, whether in the boardroom, the classroom or beyond.
And remember, you’re not alone in this journey. Venngage’s Case Study Creator is your trusty companion, ready to elevate your presentations from ordinary to extraordinary. So, let your confidence shine, leverage your newly acquired skills and prepare to deliver presentations that truly resonate.
Go forth and make a lasting impact!
9 Creative Case Study Presentation Examples & Templates
Learn from proven case study presentation examples and best practices how to get creative, stand out, engage your audience, excite action, and drive results.
9 minute read

helped business professionals at:

Short answer
What makes a good case study presentation?
A good case study presentation has an engaging story, a clear structure, real data, visual aids, client testimonials, and a strong call to action. It informs and inspires, making the audience believe they can achieve similar results.
Dull case studies can cost you clients.
A boring case study presentation doesn't just risk putting your audience to sleep—it can actually stifle your growth, leading to lost sales and overlooked opportunities. When your case study fails to inspire, it's your bottom line that suffers.
Interactive elements are the secret sauce for successful case study presentations.
They not only increase reader engagement by 22% but also lead to a whopping 41% more decks being read fully, proving that the winning deck is not a monologue but a conversation that involves the reader.
Benefits of including interactive elements in your case study presentation
More decks read in full
Longer average reading time
In this post, I’ll help you shape your case studies into compelling narratives that hook your audience, make your successes shine, and drive the results you're aiming for.
Let’s go!
How to create a case study presentation that drives results?
Crafting a case study presentation that truly drives results is about more than just data—it's about storytelling, engagement, and leading your audience down the sales funnel.
Here's how you can do it:
Tell a story: Each case study should follow a narrative arc. Start with the problem, introduce your solution, and showcase the results. Make it compelling and relatable.
Leverage data: Hard numbers build credibility. Use them to highlight your successes and reinforce your points.
Use visuals: Images, infographics, and videos can enhance engagement, making complex information more digestible and memorable.
Add interactive elements: Make your presentation a two-way journey. Tools like tabs and live data calculators can increase time spent on your deck by 22% and the number of full reads by 41% .
Finish with a strong call-to-action: Every good story needs a conclusion. Encourage your audience to take the next step in their buyer journey with a clear, persuasive call-to-action.
Here's a visual representation of what a successful case study presentation should do:

How to write an engaging case study presentation?
Creating an engaging case study presentation involves strategic storytelling, understanding your audience, and sparking action. In this guide, I'll cover the essentials to help you write a compelling narrative that drives results.
What is the best format for a business case study presentation?
4 best format types for a business case study presentation:
- Problem-solution case study
- Before-and-after case study
- Success story case study
- Interview style case study
Each style has unique strengths, so pick one that aligns best with your story and audience. For a deeper dive into these formats, check out our detailed blog post on case study format types .
I also recommend watching this video breaking down the 9-step process for writing a case study:

What to include in a case study presentation?
An effective case study presentation contains 7 key elements:
- Introduction
- Company overview
- The problem/challenge
- Your solution
- Customer quotes/testimonials
To learn more about what should go in each of these sections, check out our post on what is a case study .
How to write a compelling narrative for your case study presentation?
Storytelling is the heart of an engaging case study presentation. It involves more than just stringing events together. You should weave an emotional journey that your audience can relate to.
Begin with the challenge —illustrate the magnitude of the problem that was faced. Then, introduce your solution as the hero that comes to the rescue.
As you progress, ensure your narrative highlights the transformative journey from the problem state to the successful outcome.
Here’s our recommended storyline framework:
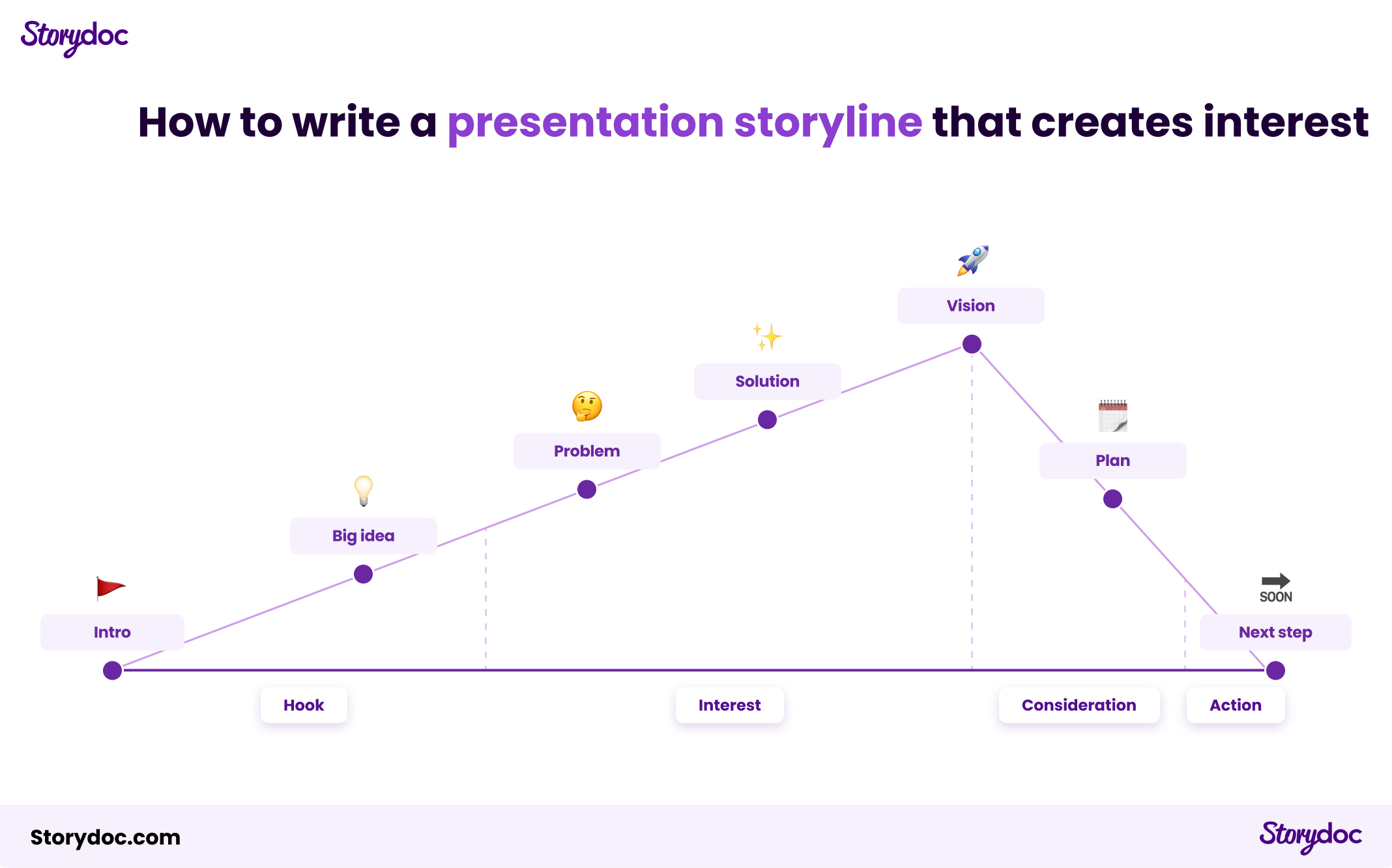
How to motivate readers to take action?
Based on BJ Fogg's behavior model , successful motivation involves 3 components:
Motivation is all about highlighting the benefits. Paint a vivid picture of the transformative results achieved using your solution. Use compelling data and emotive testimonials to amplify the desire for similar outcomes, therefore boosting your audience's motivation.
Ability refers to making the desired action easy to perform. Show how straightforward it is to implement your solution. Use clear language, break down complex ideas, and reinforce the message that success is not just possible, but also readily achievable with your offering.
Prompt is your powerful call-to-action (CTA), the spark that nudges your audience to take the next step. Ensure your CTA is clear, direct, and tied into the compelling narrative you've built. It should leave your audience with no doubt about what to do next and why they should do it.
Here’s how you can do it with Storydoc:

How to adapt your presentation for your specific audience?
Every audience is different, and a successful case study presentation speaks directly to its audience's needs, concerns, and desires.
Understanding your audience is crucial. This involves researching their pain points, their industry jargon, their ambitions, and their fears.
Then, tailor your presentation accordingly. Highlight how your solution addresses their specific problems. Use language and examples they're familiar with. Show them how your product or service can help them reach their goals.
A case study presentation that's tailor-made for its audience is not just a presentation—it's a conversation that resonates, engages, and convinces.
How to design a great case study presentation?
A powerful case study presentation is not only about the story you weave—it's about the visual journey you create.
Let's navigate through the design strategies that can transform your case study presentation into a gripping narrative.
Add interactive elements
Static design has long been the traditional route for case study presentations—linear, unchanging, a one-size-fits-all solution.
However, this has been a losing approach for a while now. Static content is killing engagement, but interactive design will bring it back to life.
It invites your audience into an evolving, immersive experience, transforming them from passive onlookers into active participants.
Which of these presentations would you prefer to read?

Use narrated content design (scrollytelling)
Scrollytelling combines the best of scrolling and storytelling. This innovative approach offers an interactive narrated journey controlled with a simple scroll.
It lets you break down complex content into manageable chunks and empowers your audience to control their reading pace.
To make this content experience available to everyone, our founder, Itai Amoza, collaborated with visualization scientist Prof. Steven Franconeri to incorporate scrollytelling into Storydoc.
This collaboration led to specialized storytelling slides that simplify content and enhance engagement (which you can find and use in Storydoc).
Here’s an example of Storydoc scrollytelling:

Bring your case study to life with multimedia
Multimedia brings a dynamic dimension to your presentation. Video testimonials lend authenticity and human connection. Podcast interviews add depth and diversity, while live graphs offer a visually captivating way to represent data.
Each media type contributes to a richer, more immersive narrative that keeps your audience engaged from beginning to end.
Prioritize mobile-friendly design
In an increasingly mobile world, design must adapt. Avoid traditional, non-responsive formats like PPT, PDF, and Word.
Opt for a mobile-optimized design that guarantees your presentation is always at its best, regardless of the device.
As a significant chunk of case studies are opened on mobile, this ensures wider accessibility and improved user experience , demonstrating respect for your audience's viewing preferences.
Here’s what a traditional static presentation looks like as opposed to a responsive deck:

Streamline the design process
Creating a case study presentation usually involves wrestling with a website builder.
It's a dance that often needs several partners - designers to make it look good, developers to make it work smoothly, and plenty of time to bring it all together.
Building, changing, and personalizing your case study can feel like you're climbing a mountain when all you need is to cross a hill.
By switching to Storydoc’s interactive case study creator , you won’t need a tech guru or a design whizz, just your own creativity.
You’ll be able to create a customized, interactive presentation for tailored use in sales prospecting or wherever you need it without the headache of mobilizing your entire team.
Storydoc will automatically adjust any change to your presentation layout, so you can’t break the design even if you tried.

Case study presentation examples that engage readers
Let’s take a deep dive into some standout case studies.
These examples go beyond just sharing information – they're all about captivating and inspiring readers. So, let’s jump in and uncover the secret behind what makes them so effective.
What makes this deck great:
- A video on the cover slide will cause 32% more people to interact with your case study .
- The running numbers slide allows you to present the key results your solution delivered in an easily digestible way.
- The ability to include 2 smart CTAs gives readers the choice between learning more about your solution and booking a meeting with you directly.
Light mode case study
- The ‘read more’ button is perfect if you want to present a longer case without overloading readers with walls of text.
- The timeline slide lets you present your solution in the form of a compelling narrative.
- A combination of text-based and visual slides allows you to add context to the main insights.
Marketing case study
- Tiered slides are perfect for presenting multiple features of your solution, particularly if they’re relevant to several use cases.
- Easily customizable slides allow you to personalize your case study to specific prospects’ needs and pain points.
- The ability to embed videos makes it possible to show your solution in action instead of trying to describe it purely with words.
UX case study
- Various data visualization components let you present hard data in a way that’s easier to understand and follow.
- The option to hide text under a 'Read more' button is great if you want to include research findings or present a longer case study.
- Content segmented using tabs , which is perfect if you want to describe different user research methodologies without overwhelming your audience.
Business case study
- Library of data visualization elements to choose from comes in handy for more data-heavy case studies.
- Ready-to-use graphics and images which can easily be replaced using our AI assistant or your own files.
- Information on the average reading time in the cover reduces bounce rate by 24% .
Modern case study
- Dynamic variables let you personalize your deck at scale in just a few clicks.
- Logo placeholder that can easily be replaced with your prospect's logo for an added personal touch.
- Several text placeholders that can be tweaked to perfection with the help of our AI assistant to truly drive your message home.
Real estate case study
- Plenty of image placeholders that can be easily edited in a couple of clicks to let you show photos of your most important listings.
- Data visualization components can be used to present real estate comps or the value of your listings for a specific time period.
- Interactive slides guide your readers through a captivating storyline, which is key in a highly-visual industry like real estate .
Medical case study
- Image and video placeholders are perfect for presenting your solution without relying on complex medical terminology.
- The ability to hide text under an accordion allows you to include research or clinical trial findings without overwhelming prospects with too much information.
- Clean interactive design stands out in a sea of old-school medical case studies, making your deck more memorable for prospective clients.
Dark mode case study
- The timeline slide is ideal for guiding readers through an attention-grabbing storyline or explaining complex processes.
- Dynamic layout with multiple image and video placeholders that can be replaced in a few clicks to best reflect the nature of your business.
- Testimonial slides that can easily be customized with quotes by your past customers to legitimize your solution in the eyes of prospects.
Grab a case study presentation template
Creating an effective case study presentation is not just about gathering data and organizing it in a document. You need to weave a narrative, create an impact, and most importantly, engage your reader.
So, why start from zero when interactive case study templates can take you halfway up?
Instead of wrestling with words and designs, pick a template that best suits your needs, and watch your data transform into an engaging and inspiring story.

Hi, I'm Dominika, Content Specialist at Storydoc. As a creative professional with experience in fashion, I'm here to show you how to amplify your brand message through the power of storytelling and eye-catching visuals.
Found this post useful?
Subscribe to our monthly newsletter.
Get notified as more awesome content goes live.
(No spam, no ads, opt-out whenever)
You've just joined an elite group of people that make the top performing 1% of sales and marketing collateral.

Create your best pitch deck to date.
Stop losing opportunities to ineffective presentations. Your new amazing deck is one click away!
- - Google Chrome
Intended for healthcare professionals
- Access provided by Google Indexer
- My email alerts
- BMA member login
- Username * Password * Forgot your log in details? Need to activate BMA Member Log In Log in via OpenAthens Log in via your institution

Search form
- Advanced search
- Search responses
- Search blogs
- Writing a case report...
Writing a case report in 10 steps
- Related content
- Peer review
- Victoria Stokes , foundation year 2 doctor, trauma and orthopaedics, Basildon Hospital ,
- Caroline Fertleman , paediatrics consultant, The Whittington Hospital NHS Trust
- victoria.stokes1{at}nhs.net
Victoria Stokes and Caroline Fertleman explain how to turn an interesting case or unusual presentation into an educational report
It is common practice in medicine that when we come across an interesting case with an unusual presentation or a surprise twist, we must tell the rest of the medical world. This is how we continue our lifelong learning and aid faster diagnosis and treatment for patients.
It usually falls to the junior to write up the case, so here are a few simple tips to get you started.
First steps
Begin by sitting down with your medical team to discuss the interesting aspects of the case and the learning points to highlight. Ideally, a registrar or middle grade will mentor you and give you guidance. Another junior doctor or medical student may also be keen to be involved. Allocate jobs to split the workload, set a deadline and work timeframe, and discuss the order in which the authors will be listed. All listed authors should contribute substantially, with the person doing most of the work put first and the guarantor (usually the most senior team member) at the end.
Getting consent
Gain permission and written consent to write up the case from the patient or parents, if your patient is a child, and keep a copy because you will need it later for submission to journals.
Information gathering
Gather all the information from the medical notes and the hospital’s electronic systems, including copies of blood results and imaging, as medical notes often disappear when the patient is discharged and are notoriously difficult to find again. Remember to anonymise the data according to your local hospital policy.
Write up the case emphasising the interesting points of the presentation, investigations leading to diagnosis, and management of the disease/pathology. Get input on the case from all members of the team, highlighting their involvement. Also include the prognosis of the patient, if known, as the reader will want to know the outcome.
Coming up with a title
Discuss a title with your supervisor and other members of the team, as this provides the focus for your article. The title should be concise and interesting but should also enable people to find it in medical literature search engines. Also think about how you will present your case study—for example, a poster presentation or scientific paper—and consider potential journals or conferences, as you may need to write in a particular style or format.
Background research
Research the disease/pathology that is the focus of your article and write a background paragraph or two, highlighting the relevance of your case report in relation to this. If you are struggling, seek the opinion of a specialist who may know of relevant articles or texts. Another good resource is your hospital library, where staff are often more than happy to help with literature searches.
How your case is different
Move on to explore how the case presented differently to the admitting team. Alternatively, if your report is focused on management, explore the difficulties the team came across and alternative options for treatment.
Finish by explaining why your case report adds to the medical literature and highlight any learning points.
Writing an abstract
The abstract should be no longer than 100-200 words and should highlight all your key points concisely. This can be harder than writing the full article and needs special care as it will be used to judge whether your case is accepted for presentation or publication.
Discuss with your supervisor or team about options for presenting or publishing your case report. At the very least, you should present your article locally within a departmental or team meeting or at a hospital grand round. Well done!
Competing interests: We have read and understood BMJ’s policy on declaration of interests and declare that we have no competing interests.
Overview and General Information about Oral Presentation
- Daily Presentations During Work Rounds
- The New Patient Presentation
- The Holdover Admission Presentation
- Outpatient Clinic Presentations
- The structure of presentations varies from service to service (e.g. medicine vs. surgery), amongst subspecialties, and between environments (inpatient vs. outpatient). Applying the correct style to the right setting requires that the presenter seek guidance from the listeners at the outset.
- Time available for presenting is rather short, which makes the experience more stressful.
- Individual supervisors (residents, faculty) often have their own (sometimes quirky) preferences regarding presentation styles, adding another layer of variability that the presenter has to manage.
- Students are evaluated/judged on the way in which they present, with faculty using this as one way of gauging a student’s clinical knowledge.
- Done well, presentations promote efficient, excellent care. Done poorly, they promote tedium, low morale, and inefficiency.
General Tips:
- Practice, Practice, Practice! Do this on your own, with colleagues, and/or with anyone who will listen (and offer helpful commentary) before you actually present in front of other clinicians. Speaking "on-the-fly" is difficult, as rapidly organizing and delivering information in a clear and concise fashion is not a naturally occurring skill.
- Immediately following your presentations, seek feedback from your listeners. Ask for specifics about what was done well and what could have been done better – always with an eye towards gaining information that you can apply to improve your performance the next time.
- Listen to presentations that are done well – ask yourself, “Why was it good?” Then try to incorporate those elements into your own presentations.
- Listen to presentations that go poorly – identify the specific things that made it ineffective and avoid those pitfalls when you present.
- Effective presentations require that you have thought through the case beforehand and understand the rationale for your conclusions and plan. This, in turn, requires that you have a good grasp of physiology, pathology, clinical reasoning and decision-making - pushing you to read, pay attention, and in general acquire more knowledge.
- Think about the clinical situation in which you are presenting so that you can provide a summary that is consistent with the expectations of your audience. Work rounds, for example, are clearly different from conferences and therefore mandate a different style of presentation.
- Presentations are the way in which we tell medical stories to one another. When you present, ask yourself if you’ve described the story in an accurate way. Will the listener be able to “see” the patient the same way that you do? Can they come to the correct conclusions? If not, re-calibrate.
- It's O.K. to use notes, though the oral presentation should not simply be reduced to reading the admission note – rather, it requires appropriate editing/shortening.
- In general, try to give your presentations on a particular service using the same order and style for each patient, every day. Following a specific format makes it easier for the listener to follow, as they know what’s coming and when they can expect to hear particular information. Additionally, following a standardized approach makes it easier for you to stay organized, develop a rhythm, and lessens the chance that you’ll omit elements.
Specific types of presentations
There are a number of common presentation-types, each with its own goals and formats. These include:
- Daily presentations during work rounds for patients known to a service.
- Newly admitted patients, where you were the clinician that performed the H&P.
- Newly admitted patients that were “handed off” to the team in the morning, such that the H&P was performed by others.
- Outpatient clinic presentations, covering several common situations.
Key elements of each presentation type are described below. Examples of how these would be applied to most situations are provided in italics. The formats are typical of presentations done for internal medicine services and clinics.
Note that there is an acceptable range of how oral presentations can be delivered. Ultimately, your goal is to tell the correct story, in a reasonable amount of time, so that the right care can be delivered. Nuances in the order of presentation, what to include, what to omit, etc. are relatively small points. Don’t let the pursuit of these elements distract you or create undue anxiety.
Daily presentations during work rounds of patients that you’re following:
- Organize the presenter (forces you to think things through)
- Inform the listener(s) of 24 hour events and plan moving forward
- Promote focused discussion amongst your listeners and supervisors
- Opportunity to reassess plan, adjust as indicated
- Demonstrate your knowledge and engagement in the care of the patient
- Rapid (5 min) presentation of the key facts
Key features of presentation:
- Opening one liner: Describe who the patient is, number of days in hospital, and their main clinical issue(s).
- 24-hour events: Highlighting changes in clinical status, procedures, consults, etc.
- Subjective sense from the patient about how they’re feeling, vital signs (ranges), and key physical exam findings (highlighting changes)
- Relevant labs (highlighting changes) and imaging
- Assessment and Plan : Presented by problem or organ systems(s), using as many or few as are relevant. Early on, it’s helpful to go through the main categories in your head as a way of making sure that you’re not missing any relevant areas. The broad organ system categories include (presented here head-to-toe): Neurological; Psychiatric; Cardiovascular; Pulmonary; Gastrointestinal; Renal/Genitourinary; Hematologic/Oncologic; Endocrine/Metabolic; Infectious; Tubes/lines/drains; Disposition.
Example of a daily presentation for a patient known to a team:
- Opening one liner: This is Mr. Smith, a 65 year old man, Hospital Day #3, being treated for right leg cellulitis
- MRI of the leg, negative for osteomyelitis
- Evaluation by Orthopedics, who I&D’d a superficial abscess in the calf, draining a moderate amount of pus
- Patient appears well, states leg is feeling better, less painful
- T Max 101 yesterday, T Current 98; Pulse range 60-80; BP 140s-160s/70-80s; O2 sat 98% Room Air
- Ins/Outs: 3L in (2 L NS, 1 L po)/Out 4L urine
- Right lower extremity redness now limited to calf, well within inked lines – improved compared with yesterday; bandage removed from the I&D site, and base had small amount of purulence; No evidence of fluctuance or undrained infection.
- Creatinine .8, down from 1.5 yesterday
- WBC 8.7, down from 14
- Blood cultures from admission still negative
- Gram stain of pus from yesterday’s I&D: + PMNS and GPCs; Culture pending
- MRI lower extremity as noted above – negative for osteomyelitis
- Continue Vancomycin for today
- Ortho to reassess I&D site, though looks good
- Follow-up on cultures: if MRSA, will transition to PO Doxycycline; if MSSA, will use PO Dicloxacillin
- Given AKI, will continue to hold ace-inhibitor; will likely wait until outpatient follow-up to restart
- Add back amlodipine 5mg/d today
- Hep lock IV as no need for more IVF
- Continue to hold ace-I as above
- Wound care teaching with RNs today – wife capable and willing to assist. She’ll be in this afternoon.
- Set up follow-up with PMD to reassess wound and cellulitis within 1 week
The Brand New Patient (admitted by you)
- Provide enough information so that the listeners can understand the presentation and generate an appropriate differential diagnosis.
- Present a thoughtful assessment
- Present diagnostic and therapeutic plans
- Provide opportunities for senior listeners to intervene and offer input
- Chief concern: Reason why patient presented to hospital (symptom/event and key past history in one sentence). It often includes a limited listing of their other medical conditions (e.g. diabetes, hypertension, etc.) if these elements might contribute to the reason for admission.
- The history is presented highlighting the relevant events in chronological order.
- 7 days ago, the patient began to notice vague shortness of breath.
- 5 days ago, the breathlessness worsened and they developed a cough productive of green sputum.
- 3 days ago his short of breath worsened to the point where he was winded after walking up a flight of stairs, accompanied by a vague right sided chest pain that was more pronounced with inspiration.
- Enough historical information has to be provided so that the listener can understand the reasons that lead to admission and be able to draw appropriate clinical conclusions.
- Past history that helps to shed light on the current presentation are included towards the end of the HPI and not presented later as “PMH.” This is because knowing this “past” history is actually critical to understanding the current complaint. For example, past cardiac catheterization findings and/or interventions should be presented during the HPI for a patient presenting with chest pain.
- Where relevant, the patient's baseline functional status is described, allowing the listener to understand the degree of impairment caused by the acute medical problem(s).
- It should be explicitly stated if a patient is a poor historian, confused or simply unaware of all the details related to their illness. Historical information obtained from family, friends, etc. should be described as such.
- Review of Systems (ROS): Pertinent positive and negative findings discovered during a review of systems are generally incorporated at the end of the HPI. The listener needs this information to help them put the story in appropriate perspective. Any positive responses to a more inclusive ROS that covers all of the other various organ systems are then noted. If the ROS is completely negative, it is generally acceptable to simply state, "ROS negative.”
- Other Past Medical and Surgical History (PMH/PSH): Past history that relates to the issues that lead to admission are typically mentioned in the HPI and do not have to be repeated here. That said, selective redundancy (i.e. if it’s really important) is OK. Other PMH/PSH are presented here if relevant to the current issues and/or likely to affect the patient’s hospitalization in some way. Unrelated PMH and PSH can be omitted (e.g. if the patient had their gall bladder removed 10y ago and this has no bearing on the admission, then it would be appropriate to leave it out). If the listener really wants to know peripheral details, they can read the admission note, ask the patient themselves, or inquire at the end of the presentation.
- Medications and Allergies: Typically all meds are described, as there’s high potential for adverse reactions or drug-drug interactions.
- Family History: Emphasis is placed on the identification of illnesses within the family (particularly among first degree relatives) that are known to be genetically based and therefore potentially heritable by the patient. This would include: coronary artery disease, diabetes, certain cancers and autoimmune disorders, etc. If the family history is non-contributory, it’s fine to say so.
- Social History, Habits, other → as relates to/informs the presentation or hospitalization. Includes education, work, exposures, hobbies, smoking, alcohol or other substance use/abuse.
- Sexual history if it relates to the active problems.
- Vital signs and relevant findings (or their absence) are provided. As your team develops trust in your ability to identify and report on key problems, it may become acceptable to say “Vital signs stable.”
- Note: Some listeners expect students (and other junior clinicians) to describe what they find in every organ system and will not allow the presenter to say “normal.” The only way to know what to include or omit is to ask beforehand.
- Key labs and imaging: Abnormal findings are highlighted as well as changes from baseline.
- Summary, assessment & plan(s) Presented by problem or organ systems(s), using as many or few as are relevant. Early on, it’s helpful to go through the main categories in your head as a way of making sure that you’re not missing any relevant areas. The broad organ system categories include (presented here head-to-toe): Neurological; Psychiatric; Cardiovascular; Pulmonary; Gastrointestinal; Renal/Genitourinary; Hematologic/Oncologic; Endocrine/Metabolic; Infectious; Tubes/lines/drains; Disposition.
- The assessment and plan typically concludes by mentioning appropriate prophylactic considerations (e.g. DVT prevention), code status and disposition.
- Chief Concern: Mr. H is a 50 year old male with AIDS, on HAART, with preserved CD4 count and undetectable viral load, who presents for the evaluation of fever, chills and a cough over the past 7 days.
- Until 1 week ago, he had been quite active, walking up to 2 miles a day without feeling short of breath.
- Approximately 1 week ago, he began to feel dyspneic with moderate activity.
- 3 days ago, he began to develop subjective fevers and chills along with a cough productive of red-green sputum.
- 1 day ago, he was breathless after walking up a single flight of stairs and spent most of the last 24 hours in bed.
- Diagnosed with HIV in 2000, done as a screening test when found to have gonococcal urethritis
- Was not treated with HAART at that time due to concomitant alcohol abuse and non-adherence.
- Diagnosed and treated for PJP pneumonia 2006
- Diagnosed and treated for CMV retinitis 2007
- Became sober in 2008, at which time interested in HAART. Started on Atripla, a combination pill containing: Efavirenz, Tonofovir, and Emtricitabine. He’s taken it ever since, with no adverse effects or issues with adherence. Receives care thru Dr. Smiley at the University HIV clinic.
- CD4 count 3 months ago was 400 and viral load was undetectable.
- He is homosexual though he is currently not sexually active. He has never used intravenous drugs.
- He has no history of asthma, COPD or chronic cardiac or pulmonary condition. No known liver disease. Hepatitis B and C negative. His current problem seems different to him then his past episode of PJP.
- Review of systems: negative for headache, photophobia, stiff neck, focal weakness, chest pain, abdominal pain, diarrhea, nausea, vomiting, urinary symptoms, leg swelling, or other complaints.
- Hypertension x 5 years, no other known vascular disease
- Gonorrhea as above
- Alcohol abuse above and now sober – no known liver disease
- No relevant surgeries
- Atripla, 1 po qd
- Omeprazole 20 mg, 1 PO, qd
- Lisinopril 20mg, qd
- Naprosyn 250 mg, 1-2, PO, BID PRN
- No allergies
- Both of the patient's parents are alive and well (his mother is 78 and father 80). He has 2 brothers, one 45 and the other 55, who are also healthy. There is no family history of heart disease or cancer.
- Patient works as an accountant for a large firm in San Diego. He lives alone in an apartment in the city.
- Smokes 1 pack of cigarettes per day and has done so for 20 years.
- No current alcohol use. Denies any drug use.
- Sexual History as noted above; has sex exclusively with men, last partner 6 months ago.
- Seated on a gurney in the ER, breathing through a face-mask oxygen delivery system. Breathing was labored and accessory muscles were in use. Able to speak in brief sentences, limited by shortness of breath
- Vital signs: Temp 102 F, Pulse 90, BP 150/90, Respiratory Rate 26, O2 Sat (on 40% Face Mask) 95%
- HEENT: No thrush, No adenopathy
- Lungs: Crackles and Bronchial breath sounds noted at right base. E to A changes present. No wheezing or other abnormal sounds noted over any other area of the lung. Dullness to percussion was also appreciated at the right base.
- Cardiac: JVP less than 5 cm; Rhythm was regular. Normal S1 and S2. No murmurs or extra heart sounds noted.
- Abdomen and Genital exams: normal
- Extremities: No clubbing, cyanosis or edema; distal pulses 2+ and equal bilaterally.
- Skin: no eruptions noted.
- Neurological exam: normal
- WBC 18 thousand with 10% bands;
- Normal Chem 7 and LFTs.
- Room air blood gas: pH of 7.47/ PO2 of 55/PCO2 of 30.
- Sputum gram stain remarkable for an abundance of polys along with gram positive diplococci.
- CXR remarkable for dense right lower lobe infiltrate without effusion.
- Monitored care unit, with vigilance for clinical deterioration.
- Hypertension: given significant pneumonia and unclear clinical direction, will hold lisinopril. If BP > 180 and or if clear not developing sepsis, will consider restarting.
- Low molecular weight heparin
- Code Status: Wishes to be full code full care, including intubation and ICU stay if necessary. Has good quality of life and hopes to return to that functional level. Wishes to reconsider if situation ever becomes hopeless. Older brother Tom is surrogate decision maker if the patient can’t speak for himself. Tom lives in San Diego and we have his contact info. He is aware that patient is in the hospital and plans on visiting later today or tomorrow.
- Expected duration of hospitalization unclear – will know more based on response to treatment over next 24 hours.
The holdover admission (presenting data that was generated by other physicians)
- Handoff admissions are very common and present unique challenges
- Understand the reasons why the patient was admitted
- Review key history, exam, imaging and labs to assure that they support the working diagnostic and therapeutic plans
- Does the data support the working diagnosis?
- Do the planned tests and consults make sense?
- What else should be considered (both diagnostically and therapeutically)?
- This process requires that the accepting team thoughtfully review their colleagues efforts with a critical eye – which is not disrespectful but rather constitutes one of the main jobs of the accepting team and is a cornerstone of good care *Note: At some point during the day (likely not during rounds), the team will need to verify all of the data directly with the patient.
- 8-10 minutes
- Chief concern: Reason for admission (symptom and/or event)
- Temporally presented bullets of events leading up to the admission
- Review of systems
- Relevant PMH/PSH – historical information that might affect the patient during their hospitalization.
- Meds and Allergies
- Family and Social History – focusing on information that helps to inform the current presentation.
- Habits and exposures
- Physical exam, imaging and labs that were obtained in the Emergency Department
- Assessment and plan that were generated in the Emergency Department.
- Overnight events (i.e. what happened in the Emergency Dept. and after the patient went to their hospital room)? Responses to treatments, changes in symptoms?
- How does the patient feel this morning? Key exam findings this morning (if seen)? Morning labs (if available)?
- Assessment and Plan , with attention as to whether there needs to be any changes in the working differential or treatment plan. The broad organ system categories include (presented here head-to-toe): Neurological; Psychiatric; Cardiovascular; Pulmonary; Gastrointestinal; Renal/Genitourinary; Hematologic/Oncologic; Endocrine/Metabolic; Infectious; Tubes/lines/drains; Disposition.
- Chief concern: 70 yo male who presented with 10 days of progressive shoulder pain, followed by confusion. He was brought in by his daughter, who felt that her father was no longer able to safely take care for himself.
- 10 days ago, Mr. X developed left shoulder pain, first noted a few days after lifting heavy boxes. He denies falls or direct injury to the shoulder.
- 1 week ago, presented to outside hospital ER for evaluation of left shoulder pain. Records from there were notable for his being afebrile with stable vitals. Exam notable for focal pain anteriorly on palpation, but no obvious deformity. Right shoulder had normal range of motion. Left shoulder reported as diminished range of motion but not otherwise quantified. X-ray negative. Labs remarkable for wbc 8, creat 2.2 (stable). Impression was that the pain was of musculoskeletal origin. Patient was provided with Percocet and told to see PMD in f/u
- Brought to our ER last night by his daughter. Pain in shoulder worse. Also noted to be confused and unable to care for self. Lives alone in the country, home in disarray, no food.
- ROS: negative for falls, prior joint or musculoskeletal problems, fevers, chills, cough, sob, chest pain, head ache, abdominal pain, urinary or bowel symptoms, substance abuse
- Hypertension
- Coronary artery disease, s/p LAD stent for angina 3 y ago, no symptoms since. Normal EF by echo 2 y ago
- Chronic kidney disease stage 3 with creatinine 1.8; felt to be secondary to atherosclerosis and hypertension
- aspirin 81mg qd, atorvastatin 80mg po qd, amlodipine 10 po qd, Prozac 20
- Allergies: none
- Family and Social: lives alone in a rural area of the county, in contact with children every month or so. Retired several years ago from work as truck driver. Otherwise non-contributory.
- Habits: denies alcohol or other drug use.
- Temp 98 Pulse 110 BP 100/70
- Drowsy though arousable; oriented to year but not day or date; knows he’s at a hospital for evaluation of shoulder pain, but doesn’t know the name of the hospital or city
- CV: regular rate and rhythm; normal s1 and s2; no murmurs or extra heart sounds.
- Left shoulder with generalized swelling, warmth and darker coloration compared with Right; generalized pain on palpation, very limited passive or active range of motion in all directions due to pain. Right shoulder appearance and exam normal.
- CXR: normal
- EKG: sr 100; nl intervals, no acute changes
- WBC 13; hemoglobin 14
- Na 134, k 4.6; creat 2.8 (1.8 baseline 4 m ago); bicarb 24
- LFTs and UA normal
- Vancomycin and Zosyn for now
- Orthopedics to see asap to aspirate shoulder for definitive diagnosis
- If aspiration is consistent with infection, will need to go to Operating Room for wash out.
- Urine electrolytes
- Follow-up on creatinine and obtain renal ultrasound if not improved
- Renal dosing of meds
- Strict Ins and Outs.
- follow exam
- obtain additional input from family to assure baseline is, in fact, normal
- Since admission (6 hours) no change in shoulder pain
- This morning, pleasant, easily distracted; knows he’s in the hospital, but not date or year
- T Current 101F Pulse 100 BP 140/80
- Ins and Outs: IVF Normal Saline 3L/Urine output 1.5 liters
- L shoulder with obvious swelling and warmth compared with right; no skin breaks; pain limits any active or passive range of motion to less than 10 degrees in all directions
- Labs this morning remarkable for WBC 10 (from 13), creatinine 2 (down from 2.8)
- Continue with Vancomycin and Zosyn for now
- I already paged Orthopedics this morning, who are en route for aspiration of shoulder, fluid for gram stain, cell count, culture
- If aspirate consistent with infection, then likely to the OR
- Continue IVF at 125/h, follow I/O
- Repeat creatinine later today
- Not on any nephrotoxins, meds renaly dosed
- Continue antibiotics, evaluation for primary source as above
- Discuss with family this morning to establish baseline; possible may have underlying dementia as well
- SC Heparin for DVT prophylaxis
- Code status: full code/full care.
Outpatient-based presentations
There are 4 main types of visits that commonly occur in an outpatient continuity clinic environment, each of which has its own presentation style and purpose. These include the following, each described in detail below.
- The patient who is presenting for their first visit to a primary care clinic and is entirely new to the physician.
- The patient who is returning to primary care for a scheduled follow-up visit.
- The patient who is presenting with an acute problem to a primary care clinic
- The specialty clinic evaluation (new or follow-up)
It’s worth noting that Primary care clinics (Internal Medicine, Family Medicine and Pediatrics) typically take responsibility for covering all of the patient’s issues, though the amount of energy focused on any one topic will depend on the time available, acuity, symptoms, and whether that issue is also followed by a specialty clinic.
The Brand New Primary Care Patient
Purpose of the presentation
- Accurately review all of the patient’s history as well as any new concerns that they might have.
- Identify health related problems that need additional evaluation and/or treatment
- Provide an opportunity for senior listeners to intervene and offer input
Key features of the presentation
- If this is truly their first visit, then one of the main reasons is typically to "establish care" with a new doctor.
- It might well include continuation of therapies and/or evaluations started elsewhere.
- If the patient has other specific goals (medications, referrals, etc.), then this should be stated as well. Note: There may well not be a "chief complaint."
- For a new patient, this is an opportunity to highlight the main issues that might be troubling/bothering them.
- This can include chronic disorders (e.g. diabetes, congestive heart failure, etc.) which cause ongoing symptoms (shortness of breath) and/or generate daily data (finger stick glucoses) that should be discussed.
- Sometimes, there are no specific areas that the patient wishes to discuss up-front.
- Review of systems (ROS): This is typically comprehensive, covering all organ systems. If the patient is known to have certain illnesses (e.g. diabetes), then the ROS should include the search for disorders with high prevalence (e.g. vascular disease). There should also be some consideration for including questions that are epidemiologically appropriate (e.g. based on age and sex).
- Past Medical History (PMH): All known medical conditions (in particular those requiring ongoing treatment) are listed, noting their duration and time of onset. If a condition is followed by a specialist or co-managed with other clinicians, this should be noted as well. If a problem was described in detail during the “acute” history, it doesn’t have to be re-stated here.
- Past Surgical History (PSH): All surgeries, along with the year when they were performed
- Medications and allergies: All meds, including dosage, frequency and over-the-counter preparations. Allergies (and the type of reaction) should be described.
- Social: Work, hobbies, exposures.
- Sexual activity – may include type of activity, number and sex of partner(s), partner’s health.
- Smoking, Alcohol, other drug use: including quantification of consumption, duration of use.
- Family history: Focus on heritable illness amongst first degree relatives. May also include whether patient married, in a relationship, children (and their ages).
- Physical Exam: Vital signs and relevant findings (or their absence).
- Key labs and imaging if they’re available. Also when and where they were obtained.
- Summary, assessment & plan(s) presented by organ system and/or problems. As many systems/problems as is necessary to cover all of the active issues that are relevant to that clinic. This typically concludes with a “health care maintenance” section, which covers age, sex and risk factor appropriate vaccinations and screening tests.
The Follow-up Visit to a Primary Care Clinic
- Organize the presenter (forces you to think things through).
- Accurately review any relevant interval health care events that might have occurred since the last visit.
- Identification of new symptoms or health related issues that might need additional evaluation and/or treatment
- If the patient has no concerns, then verification that health status is stable
- Review of medications
- Provide an opportunity for listeners to intervene and offer input
- Reason for the visit: Follow-up for whatever the patient’s main issues are, as well as stating when the last visit occurred *Note: There may well not be a “chief complaint,” as patients followed in continuity at any clinic may simply be returning for a visit as directed by their doctor.
- Events since the last visit: This might include emergency room visits, input from other clinicians/specialists, changes in medications, new symptoms, etc.
- Review of Systems (ROS): Depth depends on patient’s risk factors and known illnesses. If the patient has diabetes, then a vascular ROS would be done. On the other hand, if the patient is young and healthy, the ROS could be rather cursory.
- PMH, PSH, Social, Family, Habits are all OMITTED. This is because these facts are already known to the listener and actionable aspects have presumably been added to the problem list (presented at the end). That said, these elements can be restated if the patient has a new symptom or issue related to a historical problem has emerged.
- MEDS : A good idea to review these at every visit.
- Physical exam: Vital signs and pertinent findings (or absence there of) are mentioned.
- Lab and Imaging: The reason why these were done should be mentioned and any key findings mentioned, highlighting changes from baseline.
- Assessment and Plan: This is most clearly done by individually stating all of the conditions/problems that are being addressed (e.g. hypertension, hypothyroidism, depression, etc.) followed by their specific plan(s). If a new or acute issue was identified during the visit, the diagnostic and therapeutic plan for that concern should be described.
The Focused Visit to a Primary Care Clinic
- Accurately review the historical events that lead the patient to make the appointment.
- Identification of risk factors and/or other underlying medical conditions that might affect the diagnostic or therapeutic approach to the new symptom or concern.
- Generate an appropriate assessment and plan
- Allow the listener to comment
Key features of the presentation:
- Reason for the visit
- History of Present illness: Description of the sequence of symptoms and/or events that lead to the patient’s current condition.
- Review of Systems: To an appropriate depth that will allow the listener to grasp the full range of diagnostic possibilities that relate to the presenting problem.
- PMH and PSH: Stating only those elements that might relate to the presenting symptoms/issues.
- PE: Vital signs and key findings (or lack thereof)
- Labs and imaging (if done)
- Assessment and Plan: This is usually very focused and relates directly to the main presenting symptom(s) or issues.
The Specialty Clinic Visit
Specialty clinic visits focus on the health care domains covered by those physicians. For example, Cardiology clinics are interested in cardiovascular disease related symptoms, events, labs, imaging and procedures. Orthopedics clinics will focus on musculoskeletal symptoms, events, imaging and procedures. Information that is unrelated to these disciples will typically be omitted. It’s always a good idea to ask the supervising physician for guidance as to what’s expected to be covered in a particular clinic environment.
- Highlight the reason(s) for the visit
- Review key data
- Provide an opportunity for the listener(s) to comment
- 5-7 minutes
- If it’s a consult, state the main reason(s) that the patient was referred as well as who referred them.
- If it’s a return visit, state the reasons why the patient is being followed in the clinic and when the last visit took place
- If it’s for an acute issue, state up front what the issue is Note: There may well not be a “chief complaint,” as patients followed in continuity in any clinic may simply be returning for a return visit as directed
- For a new patient, this highlights the main things that might be troubling/bothering the patient.
- For a specialty clinic, the history presented typically relates to the symptoms and/or events that are pertinent to that area of care.
- Review of systems , focusing on those elements relevant to that clinic. For a cardiology patient, this will highlight a vascular ROS.
- PMH/PSH that helps to inform the current presentation (e.g. past cardiac catheterization findings/interventions for a patient with chest pain) and/or is otherwise felt to be relevant to that clinic environment.
- Meds and allergies: Typically all meds are described, as there is always the potential for adverse drug interactions.
- Social/Habits/other: as relates to/informs the presentation and/or is relevant to that clinic
- Family history: Focus is on heritable illness amongst first degree relatives
- Physical Exam: VS and relevant findings (or their absence)
- Key labs, imaging: For a cardiology clinic patient, this would include echos, catheterizations, coronary interventions, etc.
- Summary, assessment & plan(s) by organ system and/or problems. As many systems/problems as is necessary to cover all of the active issues that are relevant to that clinic.
- Reason for visit: Patient is a 67 year old male presenting for first office visit after admission for STEMI. He was referred by Dr. Goins, his PMD.
- The patient initially presented to the ER 4 weeks ago with acute CP that started 1 hour prior to his coming in. He was found to be in the midst of a STEMI with ST elevations across the precordial leads.
- Taken urgently to cath, where 95% proximal LAD lesion was stented
- EF preserved by Echo; Peak troponin 10
- In-hospital labs were remarkable for normal cbc, chem; LDL 170, hdl 42, nl lfts
- Uncomplicated hospital course, sent home after 3 days.
- Since home, he states that he feels great.
- Denies chest pain, sob, doe, pnd, edema, or other symptoms.
- No symptoms of stroke or TIA.
- No history of leg or calf pain with ambulation.
- Prior to this admission, he had a history of hypertension which was treated with lisinopril
- 40 pk yr smoking history, quit during hospitalization
- No known prior CAD or vascular disease elsewhere. No known diabetes, no family history of vascular disease; He thinks his cholesterol was always “a little high” but doesn’t know the numbers and was never treated with meds.
- History of depression, well treated with prozac
- Discharge meds included: aspirin, metoprolol 50 bid, lisinopril 10, atorvastatin 80, Plavix; in addition he takes Prozac for depression
- Taking all of them as directed.
- Patient lives with his wife; they have 2 grown children who are no longer at home
- Works as a computer programmer
- Smoking as above
- ETOH: 1 glass of wine w/dinner
- No drug use
- No known history of cardiovascular disease among 2 siblings or parents.
- Well appearing; BP 130/80, Pulse 80 regular, 97% sat on Room Air, weight 175lbs, BMI 32
- Lungs: clear to auscultation
- CV: s1 s2 no s3 s4 murmur
- No carotid bruits
- ABD: no masses
- Ext; no edema; distal pulses 2+
- Cath from 4 weeks ago: R dominant; 95% proximal LAD; 40% Cx.
- EF by TTE 1 day post PCI with mild Anterior Hypokinesis, EF 55%, no valvular disease, moderate LVH
- Labs of note from the hospital following cath: hgb 14, plt 240; creat 1, k 4.2, lfts normal, glucose 100, LDL 170, HDL 42.
- EKG today: SR at 78; nl intervals; nl axis; normal r wave progression, no q waves
- Plan: aspirin 81 indefinitely, Plavix x 1y
- Given nitroglycerine sublingual to have at home.
- Reviewed symptoms that would indicate another MI and what to do if occurred
- Plan: continue with current dosages of meds
- Chem 7 today to check k, creatinine
- Plan: Continue atorvastatin 80mg for life
- Smoking cessation: Doing well since discharge without adjuvant treatments, aware of supports.
- Plan: AAA screening ultrasound
How to make an oral case presentation to healthcare colleagues
The content and delivery of a patient case for education and evidence-based care discussions in clinical practice.

BSIP SA / Alamy Stock Photo
A case presentation is a detailed narrative describing a specific problem experienced by one or more patients. Pharmacists usually focus on the medicines aspect , for example, where there is potential harm to a patient or proven benefit to the patient from medication, or where a medication error has occurred. Case presentations can be used as a pedagogical tool, as a method of appraising the presenter’s knowledge and as an opportunity for presenters to reflect on their clinical practice [1] .
The aim of an oral presentation is to disseminate information about a patient for the purpose of education, to update other members of the healthcare team on a patient’s progress, and to ensure the best, evidence-based care is being considered for their management.
Within a hospital, pharmacists are likely to present patients on a teaching or daily ward round or to a senior pharmacist or colleague for the purpose of asking advice on, for example, treatment options or complex drug-drug interactions, or for referral.
Content of a case presentation
As a general structure, an oral case presentation may be divided into three phases [2] :
- Reporting important patient information and clinical data;
- Analysing and synthesising identified issues (this is likely to include producing a list of these issues, generally termed a problem list);
- Managing the case by developing a therapeutic plan.

Specifically, the following information should be included [3] :
Patient and complaint details
Patient details: name, sex, age, ethnicity.
Presenting complaint: the reason the patient presented to the hospital (symptom/event).
History of presenting complaint: highlighting relevant events in chronological order, often presented as how many days ago they occurred. This should include prior admission to hospital for the same complaint.
Review of organ systems: listing positive or negative findings found from the doctor’s assessment that are relevant to the presenting complaint.
Past medical and surgical history
Social history: including occupation, exposures, smoking and alcohol history, and any recreational drug use.
Medication history, including any drug allergies: this should include any prescribed medicines, medicines purchased over-the-counter, any topical preparations used (including eye drops, nose drops, inhalers and nasal sprays) and any herbal or traditional remedies taken.
Sexual history: if this is relevant to the presenting complaint.
Details from a physical examination: this includes any relevant findings to the presenting complaint and should include relevant observations.
Laboratory investigation and imaging results: abnormal findings are presented.
Assessment: including differential diagnosis.
Plan: including any pharmaceutical care issues raised and how these should be resolved, ongoing management and discharge planning.
Any discrepancies between the current management of the patient’s conditions and evidence-based recommendations should be highlighted and reasons given for not adhering to evidence-based medicine ( see ‘Locating the evidence’ ).
Locating the evidence
The evidence base for the therapeutic options available should always be considered. There may be local guidance available within the hospital trust directing the management of the patient’s presenting condition. Pharmacists often contribute to the development of such guidelines, especially if medication is involved. If no local guidelines are available, the next step is to refer to national guidance. This is developed by a steering group of experts, for example, the British HIV Association or the National Institute for Health and Care Excellence . If the presenting condition is unusual or rare, for example, acute porphyria, and there are no local or national guidelines available, a literature search may help locate articles or case studies similar to the case.
Giving a case presentation
Currently, there are no available acknowledged guidelines or systematic descriptions of the structure, language and function of the oral case presentation [4] and therefore there is no standard on how the skills required to prepare or present a case are taught. Most individuals are introduced to this concept at undergraduate level and then build on their skills through practice-based learning.
A case presentation is a narrative of a patient’s care, so it is vital the presenter has familiarity with the patient, the case and its progression. The preparation for the presentation will depend on what information is to be included.
Generally, oral case presentations are brief and should be limited to 5–10 minutes. This may be extended if the case is being presented as part of an assessment compared with routine everyday working ( see ‘Case-based discussion’ ). The audience should be interested in what is being said so the presenter should maintain this engagement through eye contact, clear speech and enthusiasm for the case.
It is important to stick to the facts by presenting the case as a factual timeline and not describing how things should have happened instead. Importantly, the case should always be concluded and should include an outcome of the patient’s care [5] .
An example of an oral case presentation, given by a pharmacist to a doctor, is available here .
A successful oral case presentation allows the audience to garner the right amount of patient information in the most efficient way, enabling a clinically appropriate plan to be developed. The challenge lies with the fact that the content and delivery of this will vary depending on the service, and clinical and audience setting [3] . A practitioner with less experience may find understanding the balance between sufficient information and efficiency of communication difficult, but regular use of the oral case presentation tool will improve this skill.
Tailoring case presentations to your audience
Most case presentations are not tailored to a specific audience because the same type of information will usually need to be conveyed in each case.
However, case presentations can be adapted to meet the identified learning needs of the target audience, if required for training purposes. This method involves varying the content of the presentation or choosing specific cases to present that will help achieve a set of objectives [6] . For example, if a requirement to learn about the management of acute myocardial infarction has been identified by the target audience, then the presenter may identify a case from the cardiology ward to present to the group, as opposed to presenting a patient reviewed by that person during their normal working practice.
Alternatively, a presenter could focus on a particular condition within a case, which will dictate what information is included. For example, if a case on asthma is being presented, the focus may be on recent use of bronchodilator therapy, respiratory function tests (including peak expiratory flow rate), symptoms related to exacerbation of airways disease, anxiety levels, ability to talk in full sentences, triggers to worsening of symptoms, and recent exposure to allergens. These may not be considered relevant if presenting the case on an unrelated condition that the same patient has, for example, if this patient was admitted with a hip fracture and their asthma was well controlled.
Case-based discussion
The oral case presentation may also act as the basis of workplace-based assessment in the form of a case-based discussion. In the UK, this forms part of many healthcare professional bodies’ assessment of clinical practice, for example, medical professional colleges.
For pharmacists, a case-based discussion forms part of the Royal Pharmaceutical Society (RPS) Foundation and Advanced Practice assessments . Mastery of the oral case presentation skill could provide useful preparation for this assessment process.
A case-based discussion would include a pharmaceutical needs assessment, which involves identifying and prioritising pharmaceutical problems for a particular patient. Evidence-based guidelines relevant to the specific medical condition should be used to make treatment recommendations, and a plan to monitor the patient once therapy has started should be developed. Professionalism is an important aspect of case-based discussion — issues must be prioritised appropriately and ethical and legal frameworks must be referred to [7] . A case-based discussion would include broadly similar content to the oral case presentation, but would involve further questioning of the presenter by the assessor to determine the extent of the presenter’s knowledge of the specific case, condition and therapeutic strategies. The criteria used for assessment would depend on the level of practice of the presenter but, for pharmacists, this may include assessment against the RPS Foundation or Pharmacy Frameworks .
Acknowledgement
With thanks to Aamer Safdar for providing the script for the audio case presentation.
Reading this article counts towards your CPD
You can use the following forms to record your learning and action points from this article from Pharmaceutical Journal Publications.
Your CPD module results are stored against your account here at The Pharmaceutical Journal . You must be registered and logged into the site to do this. To review your module results, go to the ‘My Account’ tab and then ‘My CPD’.
Any training, learning or development activities that you undertake for CPD can also be recorded as evidence as part of your RPS Faculty practice-based portfolio when preparing for Faculty membership. To start your RPS Faculty journey today, access the portfolio and tools at www.rpharms.com/Faculty
If your learning was planned in advance, please click:
If your learning was spontaneous, please click:
[1] Onishi H. The role of case presentation for teaching and learning activities. Kaohsiung J Med Sci 2008;24:356–360. doi: 10.1016/s1607-551x(08)70132–3
[2] Edwards JC, Brannan JR, Burgess L et al . Case presentation format and clinical reasoning: a strategy for teaching medical students. Medical Teacher 1987;9:285–292. doi: 10.3109/01421598709034790
[3] Goldberg C. A practical guide to clinical medicine: overview and general information about oral presentation. 2009. University of California, San Diego. Available from: https://meded.ecsd.edu/clinicalmed.oral.htm (accessed 5 December 2015)
[4] Chan MY. The oral case presentation: toward a performance-based rhetorical model for teaching and learning. Medical Education Online 2015;20. doi: 10.3402/meo.v20.28565
[5] McGee S. Medicine student programs: oral presentation guidelines. Learning & Scholarly Technologies, University of Washington. Available from: https://catalyst.uw.edu/workspace/medsp/30311/202905 (accessed 7 December 2015)
[6] Hays R. Teaching and Learning in Clinical Settings. 2006;425. Oxford: Radcliffe Publishing Ltd.
[7] Royal Pharmaceutical Society. Tips for assessors for completing case-based discussions. 2015. Available from: http://www.rpharms.com/help/case_based_discussion.htm (accessed 30 December 2015)
You might also be interested in…

How to demonstrate empathy and compassion in a pharmacy setting

Be more proactive to convince medics, pharmacists urged

How pharmacists can encourage patient adherence to medicines
Home Blog PowerPoint Tutorials How To Prepare and Deliver a Business Case Presentation
How To Prepare and Deliver a Business Case Presentation

No matter how junior or senior an individual is in an organization, there will always be times when they need to convince others why they should fund them, choose them, or do anything else they want them to do. Sometimes an informal, but convincing, argument is enough. Often, it isn’t. Those are the times you’ll need to prepare a business case in order to change their mind.
What is a Business Case?
A business case is a document that presents the costs, risks, and benefits of a particular initiative, justifies the investment , and pitches why decision-makers should approve of the recommendation. Students pursuing an MBA with a specialization in marketing are often asked to prepare different business case studies to improve their business forecasting and analytics skills.
Depending on your organization and endeavor, this will be anything from an informal document to a formal presentation before stakeholders. Regardless of the format, a business case aims to convince people if a project or initiative is worth investing in and why one particular approach is better than others.
A Business Case Is Not a Project Proposal or a Project Plan
Don’t get a business case mixed up with a project proposal . While they have similar goals and will cover some of the same topics, they’re not quite the same thing. A project proposal focuses on what a project is, delving into many of the details like deliverables and timelines. They are also different from project plans , which explain how a project will be executed and have much more detail. A business case, on the other hand, is about why people should invest in your initiative.
When You Should Create a Business Case Presentation?
You should create a business case presentation any time you need to convince a manager or stakeholder to make a decision, where an informal conversation is not appropriate or enough.
Common reasons to create a business case presentation:
- Asking for new funding, more funding, or a continuation of funding
- Changing the scope of a project
- Starting a new project
- Requesting a policy change
- Asking for an exception to a rule
- Adding resources to a project or team
How to Create a Business Case Presentation?
While you might be eager to jump in and share the initiative you believe in, it’s a good idea to step back and make sure you prepare a solid case. The more concrete details, facts, and figures you have, the stronger your business case will be. The main sections of a business case will be the context of the situation, problem statement, opportunities, financial analysis, and solution description.
If you’ve never made a business case presentation before, consider using a business case template or try our AI presentation maker to help guide you through each step. Here’s a short summary of each of the parts of a convincing business case presentation.

Step 1. Establish Context about the Current Situation
Not all audience members will immediately know what the current situation is leading up to your initiative. Briefly lay out the background of the idea. Note that this isn’t the problem statement, which will follow.

Step 2. State the Problems
This slide is where you can impress upon your audience the importance of the problem, and therefore, why the solution you’ll soon present is necessary.
When describing the problems, think about the direct and indirect effects of the situation, as well as the internal and external implications. Include statistical analysis if you’re already seeing negative effects because of the situation.

Step 3. Evaluate Opportunities
Your solution needs to be directly related to the stated problem. Here you can list, side-by-side, the opportunities you foresee to address problems. This section is a segway from your problem to your solution.
Another way to present this section is to analyze potential causes of the previously stated problem. This would then be the step to introduce the possible approaches, before settling on the one you’ve chosen to pitch.
Step 4. Analyze Finances
The numbers are probably the most important thing on stakeholder’s minds. They can make or break your business case. Present the current financial situation and compare it to the numbers you could be achieving if they choose to fund your initiative. Additionally, emphasize the potential for increased revenue through the implementation of a recurring payment system , which can provide a steady stream of income for your business.
Step 5. Describe Solution
Now that you’ve impressed the need for a change on your audience, it’s time to propose your solution. The format of your solution description will depend on what kind of decision you’re promoting. Generally speaking, you’ll want to briefly outline what needs to be done, how it will be done, who will do it, and when it will be done. Let’s look at sample solution formats for each of the examples from the introduction:
- Convincing the project manager to add you to a team: List the skills you have, how they relate to the needs of the project, and what you’ll be able to achieve once part of that team.
- Convincing your boss to commit time to fixing a product issue: List how you can fix the issue, how much time it will take, how many resources it will take, and how much it will cost, especially when compared to the alternative.
- Convincing HR to give an employee a raise: List how much of a raise your employee will need, any other non-monetary benefits that could work, and the advantages of retaining that talent.
- Convincing the board to open a new office: This initiative is clearly much more complex than the previous examples, which means it will require a much more in-depth business case document. However, in the business case presentation, you can list the costs, forecasted ROI, resources needed, and potential benefits of opening up the satellite office.
10 Tips for Presenting Effective Business Cases
- Use unique and attention-grabbing visuals. Chances are a board of directors or management team has seen a lot of business cases. Make sure yours doesn’t look just like everyone else’s.
- Clearly state your recommendation and required investment.
- Don’t shy away from costs and risks.
- Evaluate various scenarios when presenting your solution.
- Don’t forget to practice presenting your business case when preparing the documentation.
- Use an appropriate story alongside facts and figures to hook your audience, as recommended by the Harvard Business Review .
- Don’t add too much data to your PPT slides. Remember that the rest of your details will be in the business case document.
- Involve your audience by making eye contact, mentioning specific examples they may have heard about or been involved in, and even making appropriate jokes.
- Brainstorm potential questions your audience may ask and incorporate them into your presentation.
- Prepare both a long version and a short version of your business case presentation. You might be expecting an hour to pitch your idea to stakeholders, but you might just get a few minutes while walking down the hall to an emergency meeting.
Conclusion: Do Your Initiative Justice
You have a good idea. Maybe it’s a project you really believe in, a decision that just has to be made, or a strategy that will change the game for your organization. Whatever the case, your initiative won’t get approval if you communicate it ineffectively. Create a convincing business case and present it effectively and you’ll see decisions going your way in no time.

Like this article? Please share
Business Analysis Tools, Business Presentations, Presentation, Presentation Approaches Filed under PowerPoint Tutorials
Related Articles

Filed under Business • April 4th, 2024

Consulting Presentation Slides: A Guide to PPT Consultant Tools
Get to know the best tools to craft a consulting presentation by area of interest. Fully detailed guide plus template list.

Filed under Design • March 27th, 2024
How to Make a Presentation Graph
Detailed step-by-step instructions to master the art of how to make a presentation graph in PowerPoint and Google Slides. Check it out!

Filed under Business • March 13th, 2024
Exploring the Significance of the Fit Gap Analysis (Examples + Templates)
Master the Fit Gap Analysis with this guide featuring professionally designed PPT templates and step-by-step examples.
Leave a Reply

- Free Study Planner
- Residency Consulting
- Free Resources
- Med School Blog
- 1-888-427-7737
The Ultimate Patient Case Presentation Template for Med Students
- by Neelesh Bagrodia
- Apr 06, 2024
- Reviewed by: Amy Rontal, MD

Knowing how to deliver a patient presentation is one of the most important skills to learn on your journey to becoming a physician. After all, when you’re on a medical team, you’ll need to convey all the critical information about a patient in an organized manner without any gaps in knowledge transfer.
One big caveat: opinions about the correct way to present a patient are highly personal and everyone is slightly different. Additionally, there’s a lot of variation in presentations across specialties, and even for ICU vs floor patients.
My goal with this blog is to give you the most complete version of a patient presentation, so you can tailor your presentations to the preferences of your attending and team. So, think of what follows as a model for presenting any general patient.
Here’s a breakdown of what goes into the typical patient presentation.

7 Ingredients for a Patient Case Presentation Template
1. the one-liner.
The one-liner is a succinct sentence that primes your listeners to the patient.
A typical format is: “[Patient name] is a [age] year-old [gender] with past medical history of [X] presenting with [Y].
2. The Chief Complaint
This is a very brief statement of the patient’s complaint in their own words. A common pitfall is when medical students say that the patient had a chief complaint of some medical condition (like cholecystitis) and the attending asks if the patient really used that word!
An example might be, “Patient has chief complaint of difficulty breathing while walking.”
3. History of Present Illness (HPI)
The goal of the HPI is to illustrate the story of the patient’s complaint.
I remember when I first began medical school, I had a lot of trouble determining what was relevant and ended up giving a lot of extra details. Don’t worry if you have the same issue. With time, you’ll learn which details are important.
The OPQRST Framework
In the beginning of your clinical experience, a helpful framework to use is OPQRST:
Describe when the issue started, and if it occurs during certain environmental or personal exposures.
P rovocative
Report if there are any factors that make the pain better or worse. These can be broad, like noting their shortness of breath worsened when lying flat, or their symptoms resolved during rest.
Relay how the patient describes their pain or associated symptoms. For example, does the patient have a burning versus a pressure sensation? Are they feeling weakness, stiffness, or pain?
R egion/Location
Indicate where the pain is located and if it radiates anywhere.
Talk about how bad the pain is for the patient. Typically, a 0-10 pain scale is useful to provide some objective measure.
Discuss how long the pain lasts and how often it occurs.
A Case Study
While the OPQRST framework is great when starting out, it can be limiting.
Let’s take an example where the patient is not experiencing pain and comes in with altered mental status along with diffuse jaundice of the skin and a history of chronic liver disease. You will find that certain sections of OPQRST do not apply.
In this event, the HPI is still a story, but with a different framework. Try to go in chronological order. Include relevant details like if there have been any changes in medications, diet, or bowel movements.
Pertinent Positive and Negative Symptoms
Regardless of the framework you use, the name of the game is pertinent positive and negative symptoms the patient is experiencing.
I’d like to highlight the word “pertinent.” It’s less likely the patient’s chronic osteoarthritis and its management is related to their new onset shortness of breath, but it’s still important for knowing the patient’s complete medical picture. A better place to mention these details would be in the “Past Medical History” section, and reserve the HPI portion for more pertinent history.
As you become exposed to more illness scripts, experience will teach you which parts of the history are most helpful to state. Also, as you spend more time on the wards, you will pick up on which questions are relevant and important to ask during the patient interview.
By painting a clear picture with pertinent positives and negatives during your presentation, the history will guide what may be higher or lower on the differential diagnosis.
Some other important components to add are the patient’s additional past medical/surgical history, family history, social history, medications, allergies, and immunizations.
The HEADSSS Method
Particularly, the social history is an important time to describe the patient as a complete person and understand how their life story may affect their present condition.
One way of organizing the social history is the HEADSSS method:
– H ome living situation and relationships – E ducation and employment – A ctivities and hobbies – D rug use (alcohol, tobacco, cocaine, etc.) Note frequency of use, and if applicable, be sure to add which types of alcohol consumption (like beer versus hard liquor) and forms of drug use. – S exual history (partners, STI history, pregnancy plans) – S uicidality and depression – S piritual and religious history
Again, there’s a lot of variation in presenting social history, so just follow the lead of your team. For example, it’s not always necessary/relevant to obtain a sexual history, so use your judgment of the situation.
4. Review of Symptoms
Oftentimes, most elements of this section are embedded within the HPI. If there are any additional symptoms not mentioned in the HPI, it’s appropriate to state them here.
5. Objective
Vital signs.
Some attendings love to hear all five vital signs: temperature, blood pressure (mean arterial pressure if applicable), heart rate, respiratory rate, and oxygen saturation. Others are happy with “afebrile and vital signs stable.” Just find out their preference and stick to that.
Physical Exam
This is one of the most important parts of the patient presentation for any specialty. It paints a picture of how the patient looks and can guide acute management like in the case of a rigid abdomen. As discussed in the HPI section, typically you should report pertinent positives and negatives. When you’re starting out, your attending and team may prefer for you to report all findings as part of your learning.
For example, pulmonary exam findings can be reported as: “Regular chest appearance. No abnormalities on palpation. Lungs resonant to percussion. Clear to auscultation bilaterally without crackles, rhonchi, or wheezing.”
Typically, you want to report the physical exams in a head to toe format: General Appearance, Mental Status, Neurologic, Eyes/Ears/Nose/Mouth/Neck, Cardiovascular, Pulmonary, Breast, Abdominal, Genitourinary, Musculoskeletal, and Skin. Depending on the situation, additional exams can be incorporated as applicable.
Now comes reporting pertinent positive and negative labs. Several labs are often drawn upon admission. It’s easy to fall into the trap of reading off all the labs and losing everyone’s attention. Here are some pieces of advice:
You normally can’t go wrong sticking to abnormal lab values.
One qualification is that for a patient with concern for acute coronary syndrome, reporting a normal troponin is essential. Also, stating the normalization of previously abnormal lab values like liver enzymes is important.
Demonstrate trends in lab values.
A lab value is just a single point in time and does not paint the full picture. For example, a hemoglobin of 10g/dL in a patient at 15g/dL the previous day is a lot more concerning than a patient who has been stable at 10g/dL for a week.
Try to avoid editorializing in this section.
Save your analysis of the labs for the assessment section. Again, this can be a point of personal preference. In my experience, the team typically wants the raw objective data in this section.
This is also a good place to state the ins and outs of your patient (if applicable). In some patients, these metrics are strictly recorded and are typically reported as total fluid in and out over the past day followed by the net fluid balance. For example, “1L in, 2L out, net -1L over the past 24 hours.”
6. Diagnostics/Imaging
Next, you’ll want to review any important diagnostic tests and imaging. For example, describe how the EKG and echo look in a patient presenting with chest pain or the abdominal CT scan in a patient with right lower quadrant abdominal pain.
Try to provide your own interpretation to develop your skills and then include the final impression. Also, report if a diagnostic test is still pending.
7. Assessment/Plan
This is the fun part where you get to use your critical thinking (aka doctor) skills! For the scope of this blog, we’ll review a problem-based plan.
It’s helpful to begin with a summary statement that incorporates the one-liner, presenting issue(s)/diagnosis(es), and patient stability.
Then, go through all the problems relevant to the admission. You can impress your audience by casting a wide differential diagnosis and going through the elements of your patient presentation that support one diagnosis over another.
Following your assessment, try to suggest a management plan. In a patient with congestive heart failure exacerbation, initiating a diuresis regimen and measuring strict ins/outs are good starting points.
You may even suggest a follow-up on their latest ejection fraction with an echo and check if they’re on guideline-directed medical therapy. Again, with more time on the clinical wards you’ll start to pick up on what management plan to suggest.
One pointer is to talk about all relevant problems, not just the presenting issue. For example, a patient with diabetes may need to be put on a sliding scale insulin regimen or another patient may require physical/occupational therapy. Just try to stay organized and be comprehensive.
A Note About Patient Presentation Skills
When you’re doing your first patient presentations, it’s common to feel nervous. There may be a lot of “uhs” and “ums.”
Here’s the good news: you don’t have to be perfect! You just need to make a good faith attempt and keep on going with the presentation.
With time, your confidence will build. Practice your fluency in the mirror when you have a chance. No one was born knowing medicine and everyone has gone through the same stages of learning you are!
Practice your presentation a couple times before you present to the team if you have time. Pull a resident aside if they have the bandwidth to make sure you have all the information you need.
One big piece of advice: NEVER LIE. If you don’t know a specific detail, it’s okay to say, “I’m not sure, but I can look that up.” Someone on your team can usually retrieve the information while you continue on with your presentation.
Example Patient Case Presentation Template
Here’s a blank patient case presentation template that may come in handy. You can adapt it to best fit your needs.
Chief Complaint:
History of Present Illness:
Past Medical History:
Past Surgical History:
Family History:
Social History:
Medications:
Immunizations:
Vital Signs : Temp ___ BP ___ /___ HR ___ RR ___ O2 sat ___
Physical Exam:
General Appearance:
Mental Status:
Neurological:
Eyes, Ears, Nose, Mouth, and Neck:
Cardiovascular:
Genitourinary:
Musculoskeletal:
Most Recent Labs:
Previous Labs:
Diagnostics/Imaging:
Impression/Interpretation:
Assessment/Plan:
One-line summary:
#Problem 1:
Assessment:
#Problem 2:
Final Thoughts on Patient Presentations
I hope this post demystified the patient presentation for you. Be sure to stay organized in your delivery and be flexible with the specifications your team may provide.
Something I’d like to highlight is that you may need to tailor the presentation to the specialty you’re on. For example, on OB/GYN, it’s important to include a pregnancy history. Nonetheless, the aforementioned template should set you up for success from a broad overview perspective.
Stay tuned for my next post on how to give an ICU patient presentation. And if you’d like me to address any other topics in a blog, write to me at [email protected] !
Looking for more (free!) content to help you through clinical rotations? Check out these other posts from Blueprint tutors on the Med School blog:
- How I Balanced My Clinical Rotations with Shelf Exam Studying
- How (and Why) to Use a Qbank to Prepare for USMLE Step 2
- How to Study For Shelf Exams: A Tutor’s Guide
About the Author
Hailing from Phoenix, AZ, Neelesh is an enthusiastic, cheerful, and patient tutor. He is a fourth year medical student at the Keck School of Medicine of the University of Southern California and serves as president for the Class of 2024. He is applying to surgery programs for residency. He also graduated as valedictorian of his high school and the USC Viterbi School of Engineering, obtaining a B.S. in Biomedical Engineering in 2020. He discovered his penchant for teaching when he began tutoring his friends for the SAT and ACT in the summer of 2015 out of his living room. Outside of the academic sphere, Neelesh enjoys surfing at San Onofre Beach and hiking in the Santa Monica Mountains. Twitter: @NeeleshBagrodia LinkedIn: http://www.linkedin.com/in/neelesh-bagrodia

Related Posts
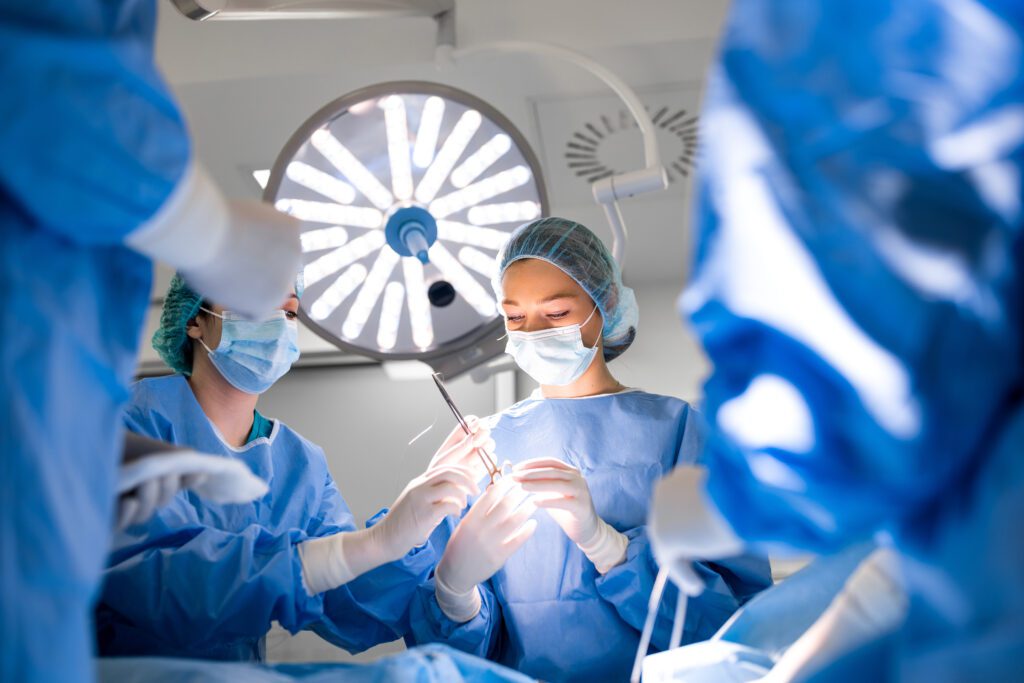
The Most Competitive Medical Specialties & How to Prepare

My Journey to Medicine: Charmian’s Story

Meet ResidencyCAS, the New OB/GYN Residency Application System
Search the blog, try blueprint med school study planner.
Create a personalized study schedule in minutes for your upcoming USMLE, COMLEX, or Shelf exam. Try it out for FREE, forever!
Could You Benefit from Tutoring?
Sign up for a free consultation to get matched with an expert tutor who fits your board prep needs
Find Your Path in Medicine
A side by side comparison of specialties created by practicing physicians, for you!
Popular Posts

Need a personalized USMLE/COMLEX study plan?

Researched by Consultants from Top-Tier Management Companies

Powerpoint Templates
Icon Bundle
Kpi Dashboard
Professional
Business Plans
Swot Analysis
Gantt Chart
Business Proposal
Marketing Plan
Project Management
Business Case
Business Model
Cyber Security
Business PPT
Digital Marketing
Digital Transformation
Human Resources
Product Management
Artificial Intelligence
Company Profile
Acknowledgement PPT
PPT Presentation
Reports Brochures
One Page Pitch
Interview PPT
All Categories
Top 7 Medical Case Presentation Templates with Samples and Examples

Sarojit Hazra
How does information expand beyond essential recollection? Facts alone can diminish in value over time. Context and implementation are crucial to form deep connections and roots. Here comes the role of case studies for clinical personnel in the medical field.
In the always-growing healthcare industry, medical case presentation is essential as it is a suggestion for new researchers. A medical case study is a report where a medical practitioner shares a patient's case. It comprises every detail related to patients. It is beneficial for describing a new medical condition, management options, or treatment for diseases.
Medical case presentations contribute significantly to the evolution of medical knowledge and research.
Case study analysis is essential for every business or industry, like the medical industry. It helps in managing the twists and turns of the industry. Want to take some ideas? Have a look at SlideTeam’s blog Case Analysis Templates .
Let us highlight some significant benefits of medical case presentation:
- Case study presentations are extremely good at depicting realistic clinical frameworks.
- It helps to enhance student participation alongside the joy of learning.
- These are ideal for sharing the latest information on the clinical landscape.
- It promotes critical thinking.
- It can also make better clinical outcomes.
If you are in the healthcare sector, another important tool is the medical dashboard. For a deeper insight, quickly take a look at Medical dashboard Templates .
Each of the slides is 100% editable and customizable. The 100% customizable nature of the templates allows you to edit your presentations. The content-ready slides give you the much-needed structure. Below, let’s explore a wide array of ready to use, content ready medical case presentation templates fit for your organization.
Template 1: Case Study on Blockchain Application in Healthcare: Medical Staff Credential Verification
Blockchain is becoming a potential solution to verify medical credentials. Though these are open to the public, they can be restricted through permissions. Are you finding it difficult to understand and implement? SlideTeam introduces this PPT Template that highlights how to operationalize medical staff verification process using blockchain technology. It explains that healthcare-based systems can also be used to verify the credentials of medical staff. Solutions-based blockchain to track the experiences of medical professionals. The PPT slides are designed with suitable icons, designs, graphs and other relevant material. Grab it quickly and draft your case study as per the client’s requirements.

Click to Download
Template 2: Cost Benefits IOT Digital Twins Implementation Use Cases in the Medical Domain
This PPT template is designed to focus on the use cases in the medical domain, including research and development, diagnosis, surgery, medical equipment, etc. The slide offers a brief description of the mentioned use cases to understand the scenario better. Use it as an essential tool and captivate your audience. Get it Now!
Template 3: Major Use Cases for Tracking Medical Assets Asset Tracking and Management IoT
Want to simplify medical complexities? The asset tracking solution is here to accompany you. It enables the medical sector to locate patients, clinicians, and medications more accurately and quickly. IoT development has made this task much more accessible by guiding you through every significant aspect of a medical asset-tracking solution. Introducing our slide exhibiting use cases of medical tools that can be tracked with IoT technology . Medical assets, including medical tools, medical equipment tracking, medications , etc., are shown in the layout with their use cases and impacts. Each topic is depicted in separate tables with appropriate icons.
Template 4: AIoT Healthcare Applications in Medical Imaging
AIoT is making the medical sector smarter and wiser to improve data management and human-machine interaction. When AIoT is applied to healthcare, enables virtual monitoring and accurate diagnosis of patients to develop a personalized patient experience. Here, we introduce our premium PPT Templates showcasing applications of Artificial Intelligence of Things (AIoT) in radiology. You can provide detailed information about remote diagnosis , personalized treatment , and real-time monitoring. Adapt it now to increase your presentation threshold and educate your audience.
Template 5: Case Study of Leading Medical Devices Manufacturing Organization
An array of disruptive themes is shaping the medical device industry, and cloud computing is one of them. Soon, cloud computing will have a more significant impact on this industry. So, for your convenience, we are presenting our slide covering a case study of blue cloud with lending medical devices manufacturing organization. It covers significant topics like client objective, problem, our solution, and results chronologically. Consisting of three essential stages, this template is excellent for educating and enticing your audience.

Template 6: IoT Technology Use Case for Medical Treatment
IoT, or the Internet of Things, is gaining significance across industries, and the medical sector is no exception. It has taken medical treatment to a new level. This custom-built PowerPoint Template exhibits the use of IoT technology in domains of the healthcare industry. It provides a digital solution for patient treatment. The key elements are primary care, acute care, virtual hospital, etc., which are depicted along with descriptions, benefits, and additional comments. Each illustration is highlighted, colored and has a relevant icon for instantaneous identification.
Template 7: IoT Medical Healthcare Technology Use Cases
The transformation of healthcare into digital healthcare has resulted in the rise of IoMT, or medical IoT . It refers to connected devices in medical healthcare and has become one of the fastest-growing industries in the IoT market. It would help if you dived deeper to manage, monitor, and preserve IoT devices in medical healthcare. This PPT presentation demonstrates uses of IoT Medical Healthcare Technology in monitoring patient health. Moreover, the slide includes remote patient monitoring, reduced waiting time, identifying chronic diseases, and drug management. Download this template design and present your case study with ultimate professionalism.
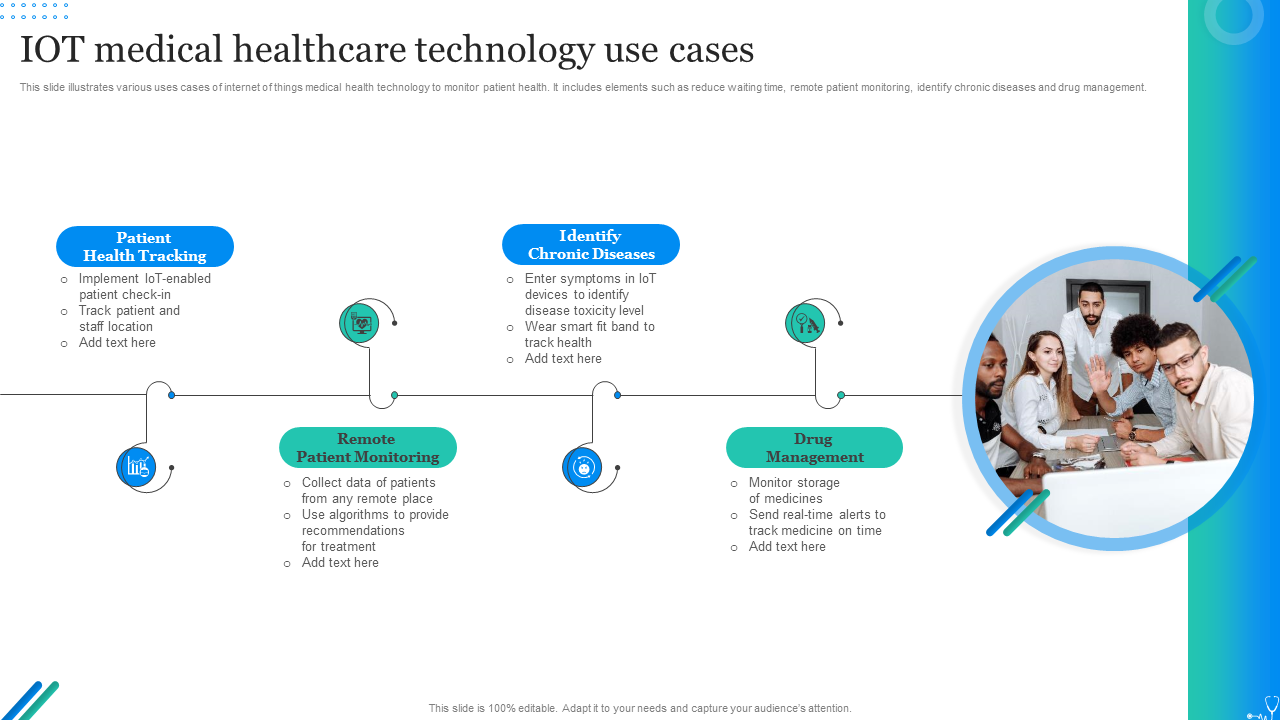
HEALTH CONSULTATION WILL BE QUICKER, SAFER AND SECURE
Case studies have a great history as an educational tool for clinicians. These are highly beneficial for nurturing deeper insights and learning. Access to such visually appealing and comprehensively presented Top 7 Medical Case Presentation Templates enables medical professionals to quickly present their patients' case studies. Be it tracking of medical assets, application of IoT in the clinical field, IoT medical healthcare technology uses, and so on, these templates serve as essential equipment in implementing all.
P.S. For perfection and success, you should dig into SlideTeam's fantastic blog, Medical Report Templates .
Related posts:
- How to Design the Perfect Service Launch Presentation [Custom Launch Deck Included]
- Quarterly Business Review Presentation: All the Essential Slides You Need in Your Deck
- [Updated 2023] How to Design The Perfect Product Launch Presentation [Best Templates Included]
- 99% of the Pitches Fail! Find Out What Makes Any Startup a Success
Liked this blog? Please recommend us

Top 10 Training Framework Templates with Examples and Samples

Top 5 Product Strategy Framework Templates with Samples and Examples
This form is protected by reCAPTCHA - the Google Privacy Policy and Terms of Service apply.

Digital revolution powerpoint presentation slides

Sales funnel results presentation layouts
3d men joinning circular jigsaw puzzles ppt graphics icons

Business Strategic Planning Template For Organizations Powerpoint Presentation Slides
Future plan powerpoint template slide

Project Management Team Powerpoint Presentation Slides

Brand marketing powerpoint presentation slides

Launching a new service powerpoint presentation with slides go to market

Agenda powerpoint slide show
Four key metrics donut chart with percentage

Engineering and technology ppt inspiration example introduction continuous process improvement

Meet our team representing in circular format

Tools for the Patient Presentation
The formal patient presentation.
- Posing the Clinical Question
- Searching the Medical Literature for EBM
Sources & Further Reading
First Aid for the Wards
Lingard L, Haber RJ. Teaching and learning communications in medicine: a rhetorical approach . Academic Medicine. 74(5):507-510 1999 May.
Lingard L, Haber RJ. What do we mean by "relevance"? A clinical and rhetorical definition with implications for teaching and learning the case-presentation format . Academic Medicine. 74(10):S124-S127.
The Oral Presentation (A Practical Guide to Clinical Medicine, UCSD School of Medicine) http://meded.ucsd.edu/clinicalmed/oral.htm
"Classically, the formal oral presentation is given in 7 minutes or less. Although it follows the same format as a written report, it is not simply regurgitation. A great presentation requires style as much as substance; your delivery must be succinct and smooth. No time should be wasted on superfluous information; one can read about such matters later in your admit note. Ideally, your presentation should be formulated so that your audience can anticipate your assessment and plan; that is, each piece of information should clue the listener into your thinking process and your most likely diagnosis." [ Le, et al, p. 15 ]
Types of Patient Presentations
New Patient
New patients get the traditional H&P with assessment and plan. Give the chief complaint and a brief and pertinent HPI. Next give important PMH, PSH, etc. The ROS is often left out, as anything important was in the HPI. The PE is reviewed. Only give pertinent positives and negatives. The assessment and plan should include what you think is wrong and, briefly, why. Then, state what you plan to do for the patient, including labs. Be sure to know why things are being done: you will be asked.
The follow-up presentation differs from the presentation of a new patient. It is an abridged presentation, perhaps referencing major patient issues that have been previously presented, but focusing on new information about these issues and/or what has changed. Give the patient’s name, age, date of admission, briefly review the present illness, physical examination and admitting diagnosis. Then report any new finding, laboratory tests, diagnostic procedures and changes in medications.
The attending physician will ask the patient’s permission to have the medical student present their case. After making the proper introductions the attending will let the patient know they may offer input or ask questions at any point. When presenting at bedside the student should try to involve the patient.
Preparing for the Presentation
There are four things you must consider before you do your oral presentation
- Occasion (setting and circumstances)
Ask yourself what do you want the presentation to do
- Present a new patient to your preceptor : the amount of detail will be determined by your preceptor. It is also likely to reflect your development and experience, with less detail being required as you progress.
- Present your patient at working or teaching rounds : the amount of detail will be determined by the customs of the group. The focus of the presentation will be influenced by the learning objectives of working responsibilities of the group.
- Request a consultant’s advice on a clinical problem : the presentation will be focused on the clinical question being posed to the consultant.
- Persuade others about a diagnosis and plan : a shorter presentation which highlights the pertinent positives and negatives that are germane to the diagnosis and/or plan being suggested.
- Enlist cooperation required for patient care : a short presentation focusing on the impact your audience can have in addressing the patient’s issues.
Preparation
- Patient evaluation : history, physical examination, review of tests, studies, procedures, and consultants’ recommendations.
- Selected reading : reference texts; to build a foundational understanding.
- Literature search : for further elucidation of any key references from selected reading, and to bring your understanding up to date, since reference text information is typically three to seven years old.
- Write-up : for oral presentation, just succinct notes to serve as a reminder or reference, since you’re not going to be reading your presentation.
Knowledge (Be prepared to answer questions about the following)
- Pathophysiology
- Complications
- Differential diagnosis
- Course of conditions
- Diagnostic tests
- Medications
- Essential Evidence Plus
Template for Oral Presentations
Chief Complaint (CC)
The opening statement should give an overview of the patient, age, sex, reason for visit and the duration of the complaint. Give marital status, race, or occupation if relevant. If your patient has a history of a major medical problem that bears strongly on the understanding of the present illness, include it. For ongoing care, give a one sentence recap of the history.
History of Present Illness (HPI)
This will be very similar to your written HPI. Present the most important problem first. If there is more than one problem, treat each separately. Present the information chronologically. Cover one system before going onto the next. Characterize the chief complaint – quality, severity, location, duration, progression, and include pertinent negatives. Items from the ROS that are unrelated to the present problem may be mentioned in passing unless you are doing a very formal presentation. When you do your first patient presentation you may be expected to go into detail. For ongoing care, present any new complaints.
Review of Systems (ROS)
Most of the ROS is incorporated at the end of the HPI. Items that are unrelated to the present problem may be briefly mentioned. For ongoing care, present only if new complaints.
Past Medical History (PMH)
Discuss other past medical history that bears directly on the current medical problem. For ongoing care, have the information available to respond to questions.
Past Surgical History
Provide names of procedures, approximate dates, indications, any relevant findings or complications, and pathology reports, if applicable. For ongoing care, have the information available to respond to questions.
Allergies/Medications
Present all current medications along with dosage, route and frequency. For the follow-up presentation just give any changes in medication. For ongoing care, note any changes.
Smoking and Alcohol (and any other substance abuse)
Note frequency and duration. For ongoing care, have the information available to respond to questions.
Social/Work History
Home, environment, work status and sexual history. For ongoing care, have the information available to respond to questions.
Family History Note particular family history of genetically based diseases. For ongoing care, have the information available to respond to questions.
Physical Exam/Labs/Other Tests
Include all significant abnormal findings and any normal findings that contribute to the diagnosis. Give a brief, general description of the patient including physical appearance. Then describe vital signs touching on each major system. Try to find out in advance how thorough you need to be for your presentation. There are times when you will be expected to give more detail on each physical finding, labs and other test results. For ongoing care, mention only further positive findings and relevant negative findings.
Assessment and Plan
Give a summary of the important aspects of the history, physical exam and formulate the differential diagnosis. Make sure to read up on the patient’s case by doing a search of the literature.
- Include only the most essential facts; but be ready to answer ANY questions about all aspects of your patient.
- Keep your presentation lively.
- Do not read the presentation!
- Expect your listeners to ask questions.
- Follow the order of the written case report.
- Keep in mind the limitation of your listeners.
- Beware of jumping back and forth between descriptions of separate problems.
- Use the presentation to build your case.
- Your reasoning process should help the listener consider a differential diagnosis.
- Present the patient as well as the illness .
- << Previous: Home
- Next: Posing the Clinical Question >>
- Last Updated: Jul 19, 2023 10:52 AM
- URL: https://rowanmed.libguides.com/tools
Featured Clinical Reviews
- Screening for Atrial Fibrillation: US Preventive Services Task Force Recommendation Statement JAMA Recommendation Statement January 25, 2022
- Evaluating the Patient With a Pulmonary Nodule: A Review JAMA Review January 18, 2022
- Download PDF
- Share X Facebook Email LinkedIn
- Permissions
The Oral Case Presentation : A Key Tool for Assessment and Teaching in Competency-Based Medical Education
- 1 Wilson Centre, University of Toronto, Toronto, Ontario, Canada
- 2 Department of Medicine, University of Toronto, Toronto, Ontario, Canada
- 3 HoPingKong Centre, University Health Network, Toronto, Ontario, Canada
Oral case presentations by trainees to supervisors are core activities in academic hospitals across all disciplines and form a key milestone in US and Canadian educational frameworks. Yet despite their widespread use, there has been limited attention devoted to developing case presentations as tools for structured teaching and assessment. In this Viewpoint, we discuss the challenges in using oral case presentations in medical education, including lack of standardization, high cognitive demands, and the role of trust between supervisor and trainee. We also articulate how, by addressing these tensions, case presentations can play an important role in competency-based education, both for assessment of clinical competence and for teaching clinical reasoning.
Read More About
Melvin L , Cavalcanti RB. The Oral Case Presentation : A Key Tool for Assessment and Teaching in Competency-Based Medical Education . JAMA. 2016;316(21):2187–2188. doi:10.1001/jama.2016.16415
Manage citations:
© 2024
Artificial Intelligence Resource Center
Cardiology in JAMA : Read the Latest
Browse and subscribe to JAMA Network podcasts!
Others Also Liked
Select your interests.
Customize your JAMA Network experience by selecting one or more topics from the list below.
- Academic Medicine
- Acid Base, Electrolytes, Fluids
- Allergy and Clinical Immunology
- American Indian or Alaska Natives
- Anesthesiology
- Anticoagulation
- Art and Images in Psychiatry
- Artificial Intelligence
- Assisted Reproduction
- Bleeding and Transfusion
- Caring for the Critically Ill Patient
- Challenges in Clinical Electrocardiography
- Climate and Health
- Climate Change
- Clinical Challenge
- Clinical Decision Support
- Clinical Implications of Basic Neuroscience
- Clinical Pharmacy and Pharmacology
- Complementary and Alternative Medicine
- Consensus Statements
- Coronavirus (COVID-19)
- Critical Care Medicine
- Cultural Competency
- Dental Medicine
- Dermatology
- Diabetes and Endocrinology
- Diagnostic Test Interpretation
- Drug Development
- Electronic Health Records
- Emergency Medicine
- End of Life, Hospice, Palliative Care
- Environmental Health
- Equity, Diversity, and Inclusion
- Facial Plastic Surgery
- Gastroenterology and Hepatology
- Genetics and Genomics
- Genomics and Precision Health
- Global Health
- Guide to Statistics and Methods
- Hair Disorders
- Health Care Delivery Models
- Health Care Economics, Insurance, Payment
- Health Care Quality
- Health Care Reform
- Health Care Safety
- Health Care Workforce
- Health Disparities
- Health Inequities
- Health Policy
- Health Systems Science
- History of Medicine
- Hypertension
- Images in Neurology
- Implementation Science
- Infectious Diseases
- Innovations in Health Care Delivery
- JAMA Infographic
- Law and Medicine
- Leading Change
- Less is More
- LGBTQIA Medicine
- Lifestyle Behaviors
- Medical Coding
- Medical Devices and Equipment
- Medical Education
- Medical Education and Training
- Medical Journals and Publishing
- Mobile Health and Telemedicine
- Narrative Medicine
- Neuroscience and Psychiatry
- Notable Notes
- Nutrition, Obesity, Exercise
- Obstetrics and Gynecology
- Occupational Health
- Ophthalmology
- Orthopedics
- Otolaryngology
- Pain Medicine
- Palliative Care
- Pathology and Laboratory Medicine
- Patient Care
- Patient Information
- Performance Improvement
- Performance Measures
- Perioperative Care and Consultation
- Pharmacoeconomics
- Pharmacoepidemiology
- Pharmacogenetics
- Pharmacy and Clinical Pharmacology
- Physical Medicine and Rehabilitation
- Physical Therapy
- Physician Leadership
- Population Health
- Primary Care
- Professional Well-being
- Professionalism
- Psychiatry and Behavioral Health
- Public Health
- Pulmonary Medicine
- Regulatory Agencies
- Reproductive Health
- Research, Methods, Statistics
- Resuscitation
- Rheumatology
- Risk Management
- Scientific Discovery and the Future of Medicine
- Shared Decision Making and Communication
- Sleep Medicine
- Sports Medicine
- Stem Cell Transplantation
- Substance Use and Addiction Medicine
- Surgical Innovation
- Surgical Pearls
- Teachable Moment
- Technology and Finance
- The Art of JAMA
- The Arts and Medicine
- The Rational Clinical Examination
- Tobacco and e-Cigarettes
- Translational Medicine
- Trauma and Injury
- Treatment Adherence
- Ultrasonography
- Users' Guide to the Medical Literature
- Vaccination
- Venous Thromboembolism
- Veterans Health
- Women's Health
- Workflow and Process
- Wound Care, Infection, Healing
- Register for email alerts with links to free full-text articles
- Access PDFs of free articles
- Manage your interests
- Save searches and receive search alerts
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Indian J Psychiatry
- v.61(6); Nov-Dec 2019
Case presentation in academic psychiatry: The clinical applications, purposes, and structure of formulation and summary
Narayana manjunatha.
Department of Psychiatry, National Institute of Mental Health and Neurosciences, Bengaluru, Karnataka, India
INTRODUCTION
Case presentation in an academic psychiatry traditionally follows one of the following three formats: 4DP format (ideal and lengthy format; described in the following section), “Case Summary” (CS) (medium format), or “Case Formulation” (CF) (short format), in order of the decreasing length, duration, and the gradual transition from the use of layman terms (in the history with a goal of layman understanding) to technical terms (in diagnostic formulation [DF] with a goal to communicate with professionals). However, the medium and short formats (CS and CF) are often preferred as a rule rather than exception routinely than the ideal and lengthy 4DP format in the area of academic psychiatry.
An ideal case presentation in academic psychiatry follows 4DP format: first is the “Detailed presentations of all clinical information,” second is the “Diagnostic summary” (DS) (it is optional, see below), third is the “Diagnostic formulation,” fourth is the Diagnosis or differential diagnosis (usually International Classification of Diseases-10 (ICD-10)/Diagnostic and Statistical Manual of Mental Disorders-5 [DSM-5]) and discussion of diagnosis with points in favor and against, and finally is the “Plan of management.” The goal of this article is to overview the clinical applications, purposes, and structure of the “formulation” and “summary” in this article with review from published literatures. Table 1 represents these formats of presentation graphically.
Graphical representation of different formats of case presentations in psychiatry
*Includes complete history, physical examination, and detailed mental status examination. DD – Differential diagnosis
CONCEPTS OF “FORMULATION” AND “SUMMARY:” SHORTCOMINGS
Despite the availability of substantial literatures, the concepts of “formulation” and “summary” are rather confusing concepts in academic psychiatry, especially with psychiatric residents. There are few shortcomings of these concepts causing this confusion. The presence of various models of formulations in psychiatric literatures is one of the reasons for this confusion such as “psychodynamic formulation,” “psychotherapeutic formulation,” and “cultural formulation.” It is essential to understand the purposes of the existing models of these psychiatric formulations. The “psychodynamic formulation” focuses on psychodynamic understanding of the problems of patients and may involve interventions with psychodynamic psychotherapy, the “psychotherapeutic formulation” aims to understand the problems of patients and helps to choose the different schools of psychotherapy, and the “cultural psychiatric formulation” focuses on understanding of the patient's problems from his/her cultural background. Lack of clarity on this pair of terminologies such as “case formulation” versus “diagnostic formulation” and “case summary” versus “diagnostic summary” in published literatures is another significant reason for confusion. Kuruvilla and Kuruvilla[ 1 ] in their article entitled “diagnostic formulation” denotes the inclusion of diagnosis (at least the differential diagnosis) and plan of management in the formulation. The author wishes to convey that “diagnostic formulation” and “case formulation” (formulating a case) are rather different concepts with different purposes. The concept “CF” denotes for formulating a case for the purpose of both diagnostic and management purposes, whereas “DF” with the term “diagnostic” denotes diagnostic point of view only (where term itself denotes diagnosis), which excludes the “plan of management.” The similar explanation is offered to differentiate “CS” and “DS.” Often, these pairs of terminology are used synonymously causing confusion. Further discussion in this article is based on the above explanations of all these four terms. However, if examiners/teachers ask to present DF, it means formulating his/her case for the purpose of diagnostic purpose, which need not include the management plan. For the sake of better clarity, the author wishes to discuss student-friendly models of formulation, summary, and diagnosis, edited by Professor David Goldberg. Along with experienced teachers, trainees themselves are involved in deriving these concepts in explaining Professor D. Goldberg's concepts which is an interesting point.
CLINICAL APPLICATION OF DIAGNOSTIC FORMULATION AND SUMMARY
Often, the choice of presentation from one of either “DS” or “DF” in academic psychiatry depends on whether the detailed clinical information is presented or not. If detailed clinical information is presented, “DS” may be skipped and proceed directly to presentation of the third step of ideal 4DP format, i.e., “DF.” In case detailed clinical information is not presented for any reasons, the case presentation may begin with “DS” and then may proceed to “DF” (however, it is optional). In either of the ways, both “DS” and “DF” are followed by the fourth step of ideal 4DP format, i.e., the “diagnosis or differential diagnosis” (usually ICD-10 and DSM 5) and discussion of diagnosis with points in favor and against, and finally is the “plan of management.”
The choice of the presentation either “DS”/“DF”, at times, depends on the availability of time with examiners/listeners/faculties. When ample of time are available, the examiners/teachers ask residents to present a detailed presentation of all clinical data in the usual 4DP format of “presenting complaint,” “history of presenting illness,” etc., followed by “DF,” and then plan of management, and this format has the minimal scope of “DS” presentation. However, whenever time is a constraint, residents shall be asked to present the “DS” without a detailed presentation of clinical data followed by with or without “DF.” In any case, psychiatric residents shall be encouraged to learn both DS and DF for any eventuality during examination.
As discussed above, the “CF” traditionally includes only the last three steps (3 rd , 4 th , and 5 th ) of 4DP format of psychiatric case presentation. This has relevance from psychodynamic explanation of psychiatric disorders. In view of the significant development in the neurobiology of psychiatric disorders in the last few decades and high dependency of making clinical diagnosis based on the current classificatory system (ICD-10 and DSM 5), the “DF” is preferred which excludes the plan of management than the “CF” as authors believe that the presentation of the “plan of management” itself is an important skill which is expected from psychiatric residents during training and examination. However, whenever a psychiatric resident is asked to present “CF,” he/she shall include the third to fifth steps of ideal format.
PURPOSE OF DIAGNOSTIC FORMULATION AND SUMMARY
The important goal of the “DF” is to facilitate the communication of clinical information of patients with another professional/s who are familiar with technical jargons (i.e., psychopathological/psychiatric terminology), whereas the purpose of “DS” is to convey the clinical information of patients to lay persons and/or nonprofessionals and comprises all the components of a DF, but in layman's terminology. The contents of DS may be used for the purpose of psychoeducation to patients and their family.
STRUCTURE OF DIAGNOSTIC FORMULATION AND SUMMARY
The purposes of “DF” and “DS” are important to understand their structure or contents. Since “DF” is targeted for professionals, the technical jargons are used in its content, whereas “DS” is targeted for lay persons or nonprofessionals, and then layman terms are used in its content. The “DF” should be quite brief to just re-orientating the listener to the salient features of the case, often just the key demographics and major diagnostic criteria described in technical terms in as less words as possible without repetition of any word/s. The technical jargons in “DF” often include the terminology of descriptive psychopathology or diagnostic points of classificatory system (ICD-10 and DSM-5). In simple words, the structure of both DF and DS is, more or less, similar in contents, but the difference lies in the use of technical terms and layman's terms, respectively, in its structure/contents. Further details of the structure of DF and DS are discussed below in the proposed format and case vignettes.
RECOMMENDED SIZE AND TIME TO PRESENT “DIAGNOSTIC FORMULATION AND “DIAGNOSTIC SUMMARY
The completed DF shall last for about 5 min, and the recommended length for a written version is not more than one side of a A4 paper when typed,[ 1 ] which is equivalent to 10 to 15 sentences, whereas the completed DS should be short enough to cover about two sides of a A4 paper when typed,[ 2 ] which should not be more than 10 min.
SUMMARY, FORMULATION, AND DIAGNOSIS: MODEL BY PROFESSOR DAVID GOLDBERG
The following paragraphs exerted in italic (without any edition to preserve the semantic) from “ The Maudsley Handbook of Practical Psychiatry ” were edited by Professor David Goldberg. The author feels that these paragraphs are important to understand the difference between the process of summary, formulation, and diagnosis. The author intentionally deleted diagnostic points and management plan from the discussion to keep focus on DF only.
A SUMMARY is a descriptive account of collected data: Objective and impartial. In contrast, a FORMULATION is a clinical opinion: Weighing up the pros and cons of conflicting evidence, that leads to a diagnostic choice. An opinion inevitably implies a subjective view point, by virtue of assigning relative importance to each piece of evidence; in doing so, both theoretical bias and past personal experience invariably come to play. No matter how accurate the final verdict, an analysis is inextricably bound up with subjective judgments and decisions. When assigning the same patient, two experts may produce two similar summaries, but two different formulations with divergent conclusions. This is the fundamental difference: A SUMMARY is a descriptive, whereas a formulation is analytical. Therefore, a summary calls for the qualities of thoroughness, restraint, and objectivity, while a formulation demands the composite skill of methodological thinking, incisive analysis and intelligent presentation.
THE SUMMARY
It is an important document which should be drawn up with care. Its purpose is to provide a concise description of all the important aspects of the case, enabling others who are unfamiliar with the patient to grasp the essential features of the problem without needing to search elsewhere for further information. The completed summary should be short enough to cover about two sides of A4 paper when typed.
THE FORMULATION
Formulating a case with clarity and precision is probably the most testing yet challenging and crucial part of a psychiatric assessment. The skills of writing a good formulation depend upon the ability to differentiate what are merely the incidental and circumstantial biographical details from what are the salient and discriminatory features and it is this that forms the cornerstone of a clinical diagnosis. Certain features are discriminatory because they support one diagnosis as more likely candidate and discount another diagnosis as less likely.
THE DIAGNOSIS AND FORMULATION
A diagnosis involves a nomothetic (literally “law-giving”) process. This means that all cases included within the identified category have one or more properties in common. By contrast, the formulation is an idiographic process (literally “picture of the individual”). This means that it includes the unique characteristics of each patient's case which are needed for the process of management. So, while nomothetic processes are the only way we can advance knowledge about a disease, we use idiographic methods to understand and study the individual.
THE FORMAT OF THE FORMULATION
The formulation follows a logical sequence.
Demographic data: Begins with name, age, occupation, and marital status of the patient.
Descriptive formulation: Describe the nature of onset,– for example, acute or insidious; the total duration of the present illness; and course; for instance, cyclic or deteriorating. Then list of the main phenomena (namely, symptoms and signs) that characterize the disorder. As you become more experienced you should try to be selective by featuring those phenomena that are most important, either because of their diagnostic specificity or because of their predominance in severity or duration. Avoids long lists of minor or transient symptoms and negative findings. These basic data are chiefly derived from history of the present illness; the mental state and physical examinations are used to determine the syndrome diagnosis in the next section. Note that this is not usually the place to bring in other aspects of the history: That comes later. If we know the diagnosis of a previous episode of mental illness, this should also be taken into account, but remember, the present disorder may not be connected and the diagnosis may be different.
Etiology: The various factors that have contributed should be evident mainly from the family and personal histories, the history of previous illness, and the premorbid personality. Try to answer two questions: Why this patient developed this particular disorder, and why has the disorder developed at this particular time?
PROPOSED FORMATS OF “DIAGNOSTIC SUMMARY” AND “DIAGNOSTIC FORMULATION”
The general formats of “DS” and “DF” are essentially similar with slight changes in order of the presentation, which aim to reduce the number of words as well as to avoid the repetition of words.
- Sociodemographic data
- Elaboration of chief complaint with focus on positive aspects with relevant negative aspects: Presenting the long list of minor or transient symptoms and negative findings is advisable in DS to differentiate in the differential diagnosis which may be avoided in DF. Treatment history also needs to be briefed here. Please note that layman terms shall be used in DS, whereas technical jargons are used in DF
- Past psychiatric and medical history: Briefly describe the symptoms of the past psychiatric disorder and then write possible name for that psychiatric disorder in DS, whereas directly write psychiatric diagnosis in DF
- Family history: Briefly describe symptoms and age of the onset of psychiatric disorder, and then write possible name of that psychiatric disorder in DS, whereas directly write psychiatric diagnosis in DF
- Personal history: Briefly describe the positive aspects of personal history in DS, whereas the use of possible technical jargon in DF is advised
- Premorbid personality: Describe briefly each headings of premorbid personality followed by impression in DS, whereas give directly the impression in DF, i.e., well-adjusted or schizoid/schizotypal/anxious avoidant/personality traits/disorder
- Physical examination: Briefly describe positive findings in DS, whereas technical comments in DF using medial jargons
- Mental Status Examination (MSE): Briefly describe positive findings first, then give impression of that finding using psychopathological terms in DS, whereas directly write technical jargons using psychopathological terms in DF. Please note here that, in case of DF, the psychopathological findings in MSE may be similar to the history of presenting illness (HOPI). In this case, mention as “concurred with HOPI findings” in order to avoid repetition of terms (see in case vignette of DF).
Note: Please note that findings from the family and personal histories, the history of previous illness, and the premorbid personality give the etiology of presentation of case. The sequence in the format of DS may be preferred in the same way as above, whereas in DF, etiology-related history such as past, family, and personal histories as well as premorbid personality may be presented before presenting complaints, which reduce the number of words by avoiding the repetition of words (please see in case vignettes of DS and DF).
CASE VIGNETTES: DEMONSTRATION OF THE STRUCTURE OF “DS “ AND “DF “
Diagnostic summary.
A 36-year-old married and postgraduation-completed male, currently working as a software professional hailing from urban-middle socioeconomic background from Bengaluru, presented with adequate and reliable information of 20-day illness of abrupt onset and continuous course characterized by overcheerfulness, hyperactivity, and unable to sit at one place, overtalkativeness, overfamiliarity, and overspending most of the time in the last 20 days and false and firm claims that he is a minister and demand respect from people in the last 12 days, with decreased need of sleep and appetite disturbance along with socio-occupational dysfunction in the absence of organicity and schizophrenic and depressive symptoms. There was a family history of episodic mental illness suggestive of bipolar disorder in first-degree relative with age of onset at about 23 years with maintaining asymptomatic with lithium prophylaxis and past history suggestive of episodic mental illness of bipolar disorder in the last 12 years with four similar manic episodes with each 3–5 months' duration and another three depressive episodes characterized by depressed mood, reduced interest, easy fatiguability, and early-morning awakening for about 6–8 months with poor medication adherence, with nil significant personal history and well-adjusted premorbid personality. No abnormality was found in physical examination. MSE reveals overfamiliarity; easily established rapport; increased tone, tempo, and volume in speech; pacing around excessive suggestive of increased psychomotor activity; expression and observation of overcheerfulness suggestive of elated mood and affect; and delusion of grandiosity of identity for the above claim with impaired judgment and partial insight (total 250 words).
Diagnostic formulation
Mr. Sri, a 36-year-old married and postgraduation-completed male, currently working as a software professional hailing from urban-middle socio-economic status from Bengaluru, with a family history of bipolar disorder in first-degree relative with maintaining remission on lithium prophylaxis, with past history of four manic episodes and three depressive episodes in last 12 years with poor medication adherence, with nil significant personal history and well-adjusted pre-morbid personality, presented with adequate and reliable information of 20-day illness of abrupt onset and continuous course with characterized by elated mood, increased psychomotor activity, inflated self-esteem, excessive and rapid speech, overfamiliarity, and delusion of grandiosity of identity in the last 12 days with severe bio-socio-occupational dysfunction. No abnormality was found in physical examination. MSE is concurred with the above psychopathology with impaired judgment and impaired insight (total 131 words).
Please note that the above case vignettes are not exclusive and minor variation/s are still possible.
The aims of CF/CS are different from that of DF/DS. CF/CS focuses on understanding of the case-as-whole, but DF/DS aims for diagnostic points of view. The clinical applications, purposes, and structure of DF and DS are different. The authors explained hypothetical explanation of case presentation in academic psychiatry, which we feel is relevant in order to reduce the confusion in minds of present and prospective psychiatric residents. The author hope that these hypothetical explanations explained here is welcomed by the community of academic psychiatry.
Financial support and sponsorship
Conflicts of interest.
There are no conflicts of interest.
Got any suggestions?
We want to hear from you! Send us a message and help improve Slidesgo
Top searches
Trending searches

12 templates

68 templates

el salvador
32 templates

41 templates

48 templates

33 templates
Clinical Case 01-2023
Clinical case 01-2023 presentation, free google slides theme, powerpoint template, and canva presentation template.
Present your clinical case to the medical community with this dynamic and engaging presentation by Slidesgo. Who said science can’t be creative and fun?
This presentation has been created combining a traditional structure with flat illustrations to get a professional and original template. We’ve selected blue as the primary color since it’s generally used to represent the healthcare sector. Besides, the typography used is understandable and readable so that you can present your content clearly. Follow the prescription of our designers and make a difference!
Features of this template
- 100% editable and easy to modify
- 19 different slides
- Available in five colors: pink, yellow, green, blue and orange
- Contains editable graphics and maps
- Includes 1000+ icons divided into 11 different themes for customizing your slides
- Designed to be used in Google Slides, Canva and PowerPoint
- 16:9 widescreen format suitable for all types of screens
- Includes information about fonts, colors, and credits of the resources used
How can I use the template?
Am I free to use the templates?
How to attribute?
Attribution required If you are a free user, you must attribute Slidesgo by keeping the slide where the credits appear. How to attribute?
Available colors.
Original Color
Related posts on our blog

How to Add, Duplicate, Move, Delete or Hide Slides in Google Slides

How to Change Layouts in PowerPoint

How to Change the Slide Size in Google Slides
Related presentations.

Premium template
Unlock this template and gain unlimited access


IMAGES
VIDEO
COMMENTS
Learn how to craft and present a powerful case study with tips, examples and tools. Find out the purpose, structure, length, format and best practices of case study presentations. Download free templates and get inspired by case study examples.
A guide on how to structure a case presentation for different clinical and teaching settings. Learn the key components of a case presentation, such as history, examination, differential diagnosis, investigations, and management, with examples and tips.
Summarize the major points of the case. Provide a limited number (e.g. 3) of takeaway points for the audience. Tailor summary and takeaway points to your audience. Critical Thinking Skills. Successful patient case presentations: Integrate disease and drug knowledge, clinical evidence, and patient factors.
Case Presentation Format Continued 2 Date of Recorded Session: Date of session to be listened to in class. Also state session XX of XX (e.g. session 7 of 8). Note the treatment setting. Counselor Name: Your name. If session is done by two or more clinicians include the name of each, noting who lead the interview and who is doing the write-up.
Learn how to write and present a business case study with a 4-step framework, tips, and examples. Find out the best format types, design tips, and how to use compelling visuals for your case study presentation.
Learn how to deliver oral case presentations for internal medicine inpatients with this comprehensive guide. Find out the core elements of a strong oral case presentation, such as opener, history of present illness, review of systems, past medical history, family history, social history, physical exam, and more.
Learn how to create engaging and effective case study presentations with Storydoc, a tool that lets you use scrollytelling, interactive elements, and data visualization. Explore 9 creative examples and templates for different formats and industries.
2. Basic principles. An oral case presentation is NOT a simple recitation of your write-up. It is a concise, edited presentation of the most essential information. A case presentation should be memorized as much as possible by your 3rd year rotations. You can refer to notes, but should not read your presentation.
6 Case Study Presentation Templates. To help you weave a captivating narrative about the effectiveness of your solution, we've put together stunning case study templates for creating your case study. These case study presentation examples cut across various use cases and industries. 1. Marketing Case Study.
Learn how to turn an interesting case or unusual presentation into an educational report with this guide from BMJ. It covers topics such as consent, information gathering, writing up, title, background research, and conclusion.
Effective presentations require that you have thought through the case beforehand and understand the rationale for your conclusions and plan. This, in turn, requires that you have a good grasp of physiology, pathology, clinical reasoning and decision-making - pushing you to read, pay attention, and in general acquire more knowledge ...
A case presentation is a narrative of a patient's care, so it is vital the presenter has familiarity with the patient, the case and its progression. ... Case presentation format and clinical reasoning: a strategy for teaching medical students. Medical Teacher 1987;9:285-292. doi: 10.3109/01421598709034790
STRUCTURE OF A CASE REPORT[1,2] Different journals have slightly different formats for case reports. It is always a good idea to read some of the target jiurnals case reports to get a general idea of the sequence and format. In general, all case reports include the following components: an abstract, an introduction, a case, and a discussion.
A. Purpose of case presentation - to concisely summarize 4 parts of your patient's presentation: (1) history, (2) physical examination, (3) laboratory results, and (4) your understanding of these findings (i.e., clinical reasoning). The oral case presentation is a story that leads to the diagnosis you have chosen. B.
When describing the problems, think about the direct and indirect effects of the situation, as well as the internal and external implications. Include statistical analysis if you're already seeing negative effects because of the situation. State the Problems Business Case PowerPoint Templates. Step 3.
CLINICAL CASE PRESENTATION ... In order to give an oral presentation, you need to compress the patient's medical illness and the physical findings into a concise recitation of the most essential facts. You need to give all of the relevant information without extraneous details so that the person reading it
7 Ingredients for a Patient Case Presentation Template 1. The One-Liner. The one-liner is a succinct sentence that primes your listeners to the patient. A typical format is: "[Patient name] is a [age] year-old [gender] with past medical history of [X] presenting with [Y]. 2. The Chief Complaint
Find free medical Google Slides and PowerPoint templates to present clinical cases in various specialties. Customize them with graphic resources and create engaging presentations for your audience.
Case studies have a great history as an educational tool for clinicians. These are highly beneficial for nurturing deeper insights and learning. Access to such visually appealing and comprehensively presented Top 7 Medical Case Presentation Templates enables medical professionals to quickly present their patients' case studies.
A clinical and rhetorical definition with implications for teaching and learning the case-presentation format. Academic Medicine. 74(10):S124-S127. ... Use the presentation to build your case. Your reasoning process should help the listener consider a differential diagnosis. Present the patient as well as the illness. << Previous: Home;
To help overcome the barriers to using the case presentation as an educational and assessment tool, 3 main steps are required. First, it is essential to delineate clear expectations of presentation format for trainees, allowing shared goals for tutor and learner, with the aim to optimize learning.
INTRODUCTION. Case presentation in an academic psychiatry traditionally follows one of the following three formats: 4DP format (ideal and lengthy format; described in the following section), "Case Summary" (CS) (medium format), or "Case Formulation" (CF) (short format), in order of the decreasing length, duration, and the gradual transition from the use of layman terms (in the history ...
This presentation has been created combining a traditional structure with flat illustrations to get a professional and original template. We've selected blue as the primary color since it's generally used to represent the healthcare sector. Besides, the typography used is understandable and readable so that you can present your content clearly.