Got any suggestions?
We want to hear from you! Send us a message and help improve Slidesgo
Top searches
Trending searches


solar eclipse
25 templates

145 templates

biochemistry
37 templates

12 templates

sunday school
65 templates

education technology
181 templates
Head Injury Symptoms and Causes
Head injury symptoms and causes presentation, free google slides theme and powerpoint template.
When it comes to presenting medical information, it's crucial to have clear and concise visuals that help educate and inform the audience. This Google Slides and PPT template offers just that when it comes to delivering a presentation on head injuries. With a simple yet effective style and decorated with helpful illustrations, this template ensures a professional and engaging experience for both the presenter and viewers. What sets it apart is the AI-generated text that's included, saving you time and effort when developing your presentation. With this easy-to-use template, you can confidently educate your audience on the symptoms and causes of head injuries.
Features of this template
- 100% editable and easy to modify
- 20 different slides to impress your audience
- Contains easy-to-edit graphics such as graphs, maps, tables, timelines and mockups
- Includes 500+ icons and Flaticon’s extension for customizing your slides
- Designed to be used in Google Slides and Microsoft PowerPoint
- 16:9 widescreen format suitable for all types of screens
- Includes information about fonts, colors, and credits of the resources used
How can I use the template?
Am I free to use the templates?
How to attribute?
Attribution required If you are a free user, you must attribute Slidesgo by keeping the slide where the credits appear. How to attribute?
Related posts on our blog.

How to Add, Duplicate, Move, Delete or Hide Slides in Google Slides

How to Change Layouts in PowerPoint

How to Change the Slide Size in Google Slides
Related presentations.

Premium template
Unlock this template and gain unlimited access


- My presentations
Auth with social network:
Download presentation
We think you have liked this presentation. If you wish to download it, please recommend it to your friends in any social system. Share buttons are a little bit lower. Thank you!
Presentation is loading. Please wait.
Injuries to the Head, Neck, and Face
Published by Roderick Boyd Modified over 5 years ago
Similar presentations
Presentation on theme: "Injuries to the Head, Neck, and Face"— Presentation transcript:

A First Aid Guide for the Youth Coach Prevention and Care of Injuries.

Sports Medicine HEAD Injuries CHAPTER 22 Vocabulary: Encephalon Meninges Cerebrospinal fluid Automatism Posttraumatic amnesia Retrograde.

Head and Face Injuries.

Treat a Casualty with a Closed Head Injury. Combat Trauma Treatment 2Head Injury Introduction Most common for individuals working in hazardous environments.

Neurological Injury Management Neurological Injury Management.

Chapter 21 Face and Throat Injuries. Chapter 21: Face and Throat Injuries 2 List the steps in the emergency medical care of the patient with soft-tissue.

Head, Face, Eyes, Ears, Nose and Throat Dekaney High School Houston, Texas.

Head Trauma.

Head Injury Terminology and Identification Sports Medicine.

HEAD AND FACE CHAPTER 22.

Injuries to the Head, Neck and Face
First Aid for Colleges and Universities 10 Edition Chapter 13 © 2012 Pearson Education, Inc. Head and Spine Injuries Slide Presentation prepared by Randall.

Athletic Injuries ATC 222 Head, Face, Eyes, Ears, Nose, and Throat Chapter 22.

Head & Neck. Cranium – protects brain. Frontal Parietal (2) Occipital Temporal (2) Facial Mandible Maxille (2) Zygomatic (2) Nasal.
Head Injuries. Objectives Know the difference between concussion, countercoup concussion, & second impact syndrome Differentiate the grades of concussions.

Closed Head Injuries in High School Athletics Kent Jason Lowry, MD Northland Orthopedic Associates.

Head Injuries Care & Prevention of Athletic Injuries Ms. Herrera ATC/L.

Ch. 23 Head and Face Head.
About project
© 2024 SlidePlayer.com Inc. All rights reserved.

- Upload Ppt Presentation
- Upload Pdf Presentation
- Upload Infographics
- User Presentation
- Related Presentations
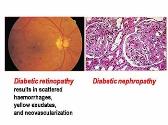
Anti-diabetic Drugs
By: drdwayn Views: 3634
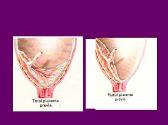
OB and GYN EMERGENCIES
By: drdwayn Views: 1740

ENDOCRINE DISORDERS in the ELDERLY - PAGETS DISEASE and ADRENAL DISEASES
By: drdwayn Views: 1084
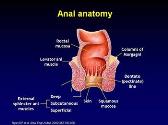
Cancers in HIV: A Growing Problem
By: drdwayn Views: 925
AHD Fundamental Neurosceience
By: drdwayn Views: 749
Malignant Peripheral Nerves Heath Tumors-MPNST
By: medhelp Views: 436
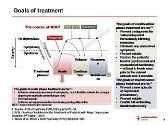
Treatment principles - Major depressive disorder
By: JenniferDwayne Views: 1233
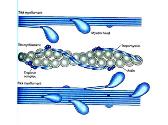

Molecular Genetics of Muscle Disorders
By: KhushbuSG Views: 352
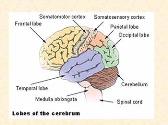
Human Body Systems-Nervous Muscles and Skeleton Systems
By: drdwayn Views: 1151
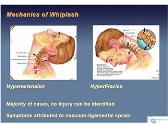
Botulinum toxin use in post traumatic cervical dystonia and head tremor
By: KhushbuSG Views: 386

- About : I am Dr. Dwayne Faulk
- Occupation : Medical Professional
- Specialty : Other Health Professionals
- Country : United States of America
HEALTH A TO Z
- Eye Disease
- Heart Attack
- Medications

Free first aid powerpoint presentations
Head Injuries
This trauma PowerPoint presentation covers head injuries. Topics include:
- Compression
- Skull fractures
- First aid management of head injuries
- AVPU and GCS
Download PowerPoint Presentation
Like us on Facebook!
Our powerpoint presentations.
- Basic First Aid Presentations
- Medical Emergencies Presentations
- Trauma Presentations
- Pediatric First Aid Presentations
- Advanced First Aid Presentations

Pin It on Pinterest
Home Collections Medical Brain Brain Injury Powerpoint Presentation
Free - Brain Injury PowerPoint Presentation and Google Slides
Brain Injury Slide For Presentation
Features of the template.
- 100% customizable slides and easy to download.
- Slides are available in different nodes & colors.
- The slides contain 16:9 and 4:3 formats.
- Easy to change the colors quickly.
- It is a well-crafted template with an instant download facility.
- It is a 100% pre-designed slide.
- The slide holds vibrant icons.
- Human Brain
- Brain Anatomy
- Human Brain Anatomy
- Brain Infographics
- Brain Function
- Neurology Human Brain
- Brain Design
- Brain Frontal Lobe
- Seven Steps Brain Infographics
- Google Slides

666+ Templates
-594.webp)
124+ Templates

Science & Research
182+ Templates

Telemedicine
40+ Templates

320+ Templates

86+ Templates
115+ Templates

43+ Templates
44+ Templates
191+ Templates
You May Also Like These PowerPoint Templates


Management of head injury
Jul 11, 2014
600 likes | 1.49k Views
Management of head injury . By : waleed alhoshan saleh aljabri wael almajed. Head injury is a leading cause of morbidity and mortality and it is the most common cause of death among all patient suffering of traumatic injury.
Share Presentation
- risk factor
- extra oculor muscle function
head injury
- gross motor function
- basilar skull
- mastoid hemotympanum

Presentation Transcript
Management of head injury By : waleedalhoshan salehaljabri waelalmajed
Head injury is a leading cause of morbidity and mortality and it is the most common cause of death among all patient suffering of traumatic injury. Motor vehicle accident are the most frequent cause of traumatic brain injury peaking in 15-24 Childe abuse is a common cause of head injury in very young infants Falls is the most common source of head injury in patient above 80 epidemiology
Head injuries include both injuries to the brain and those to other parts of the head, such as the scalp and the skull. • Brain injury is divided into primary and secondary • Primary: occurs at the time of brain injury or immediate there after eg:(skull fracture ,laceration of the brain , hemorrhage in or around the brain) • Secondary: denotes the brain response to injury eg:(cellular ischemic injury and cerebral edema ) Pathophysiology
Primary brain injury could be caused by penetrating or blunt trauma . • The brain is much more sensitive to diffuse angular application of force than focal linear one. Primary brain injury
They occur from subcellular to macroscopic level • Tissue ischemia due to the fact that Cerebral blood flow drop concededly in the early face after traumatic brain injury. • Cerebral edema occur do to cytotoxic and vasogenic mechanism and acts as an additional mass which increase intracranial pressure . Secondary brain injury
The basic management is divided into: • initial resuscitation(a,b,c,d,e) • primary neurologic survey(glasgow coma scale+ pupils+gross motor) • search for lesions that require immediate surgical management • identification and management of cerebral edema and increased intra cranial pressure. Clinical assessment
All patient with sever brain injury may require intubation purely on the basis of a reduced ability to protect the airway and maintain ventilation. • Restoring and maintaining adequate blood pressure is important • data base research demonstrate that a single episode of hypotension following brain injury doubles the risk of dying compared to patients who never had an episode.
Primary neurological survey
Glasgow coma scale
The score range from 3-15. • A score between 3-8 indicate severe brain injury . • A score between 9-12 indicate moderate brain injury. • A score between 13-15 indicate mild closed head injury.
In addition to determining the GCS the primary neurological survey include an assessment of the pupil and gross motor function . • The mass of hematoma may produce uncle herniation with unilateral pupillary dilatation and contralateral hemiparesis and these indicate a life threatening intra cranial hemorrhage is present.
Presentation varies according to the injury. A patient may present with or without neurologic deficit. • Common symptoms of head injury include: coma, confusion, drowsiness, personality change, seizures, nausea and vomiting, headache and a lucid interval, during which a patient appears conscious only to deteriorate later. • When we have a scull fracture : leaking cerebrospinal fluid and is strongly indicative of basilar skull fracture. an eye that cannot move or is deviated to one side. wounds or bruises on the scalp or face. Basilar skull fractures, those that occur at the base of the skull, are associated with Battle's sign, a subcutaneous bleed over the mastoid hemotympanum, and cerebrospinal fluid rhinorrhea and otorrhea. Sign and symptoms
All patient with moderate and sever brain injury should have a CT scan of the head . Also with mild with risk factor such as the use of anticoagulants. • Plain scull X ray is not advised as substitute for CT. • MRI maybe useful in assessing cervical and intracranial vasculature and helpful in accurate prognostication of injury outcome Diagnostic imaging
Conventional angiography ,CT scan ,and MRA are potential consideration in case of cervical intra cranial vascular injury • Conventional angiography is the gold standard and offers endovascular treatment. • After the head CT scan the clinical and radiographic information should be synthesized to formulate a plan either to operate or evaluate for intra cranial hypertension or to observe clinically for worsening of neurological status
Immediate recognition and treatment of these syndromes is essential for patient survival. • Subfalcine herniation occur when part of the cerebrum is forced from one side to an other under the falxcerebri. • There is a general correlation between the degree of Medline shift , the depression in the level of consciousness and the severity of the injury. Clinical injury pattern and herniation syndrome
Occur when the uncus of the temporal lobe is shifted medially • It can compress the oculomotor resulting in los of it’s parasympathetic function • With more sever or prolonged compression the extra oculor muscle function is also lost leading to an eye that is deviated anteriorly and laterally. • if the uncus is forced further medially it compress the cerebral peduncle producing counter lateral hemiparesis Uncal herniation
Occur when the intra cranial content particular the content of the posterior fossa are forced out of the foramen magnum • The tonsils of the cerebellum are pushed downward and compress the medulla oblongata leading to respiratory depression and death Tonsillar herniation
Bradycardia • Hypertension • Respiratory irregularity • Intubation and mechanical ventilation often obscure the respiratory part of the triad The cushing triad
Skull fracture • They are usually categorized into open or closed depressed or non depressed and basilar or convexity varieties • Depressed fracture can tear the Dura or lacerate the cortex of the brain and they are usually considered for operative repair • Skull fractures that are not depressed usually do not require repair • Basilar skull fractures can damage the the vasculature and crainial nerves and can lead to a CSF leak and meningitis • Clinically one may suspect a basilar skull fracture in the presence of battle sign or raccoon eyes Specific injuries & surgical management
The bleeding occures on the outside of the dura and collects in and expands the potential epidural space between the dura and the bone • The classic example is laceration of the middle meningeal artery by the temporal bone • The hematoma can compress the adjacent brain to the point of serious injury and death • venous epidural hematoma are less likely to produce life threatening compression • Distinguishing between the two types is location (temporal vs non temporal) ,size (small vs large) ,and the rate of exchange (slow vs fast) Epidural hematoma
The classic presentation of a tamporal epidural hematoma is a patient suffering from a blow of the temple and a brief loss of consciousness . This is fallowed by a lucid interval during which the patient appears to be neurologically well • during this time either the epidural hematoma expands slowly enough for the compensatory mechanism of the brain to maintain consciousness or the hemorrhage stops temporarily • Subsequently either due to rebleeding or exhaustion of the compensatory mechanisms a rapid decline in the level of consciousness and associated with other element of uncal herniation
Epidural hematoma has a lens shaped appearance and limited by the suture lines • CT image is also helpful in assessing the impact of the hematoma on the brain such as the degree of the midline shift or compression of the nearby structures • Management of epidual hematoma is determined by lesion size ,location and time from injury to diagnosis • Generally, an epidural hematoma more than 1cm in depth is considered for surgical management • When the diagnosis has been delayed, it is considered safe to observe patients with epidural hematoma of modest size (1cm) since the bulk of the hematoma expansion occures within the first 24-36 houres
In contrast , a 1cm thick temporal epidural hematoma in a patient only 30 minutes out from injury should be strongly considered for emergent surgical removal of the hematoma
The blood collects between the dura and the arachnoid membrane , in the potential subdural space • The force required to shear vessels in this fashion can occur with a focal blow to the head but is more common with diffuse ,rotational force applications to the brain ,as often occur in motor vehicle accidents • Most patients present with a significantly depressed level of consciousness and may have other finding related to the compressive mass of the hematoma Acute subdural hematoma
It has more of a crescent shape and there is no barrier to it’s spreading over the hemispheric surface of the brain • Associated intracerebral hemorrhage and edema is often evident beneath the acute subdural hematoma • Management of the acute subdural hematoma involves emergent operative removal by craniotomy for lesions more than 1cm thick • Acute brain swelling during the surgical procedure must be expected • Bleeding source usually difficult to stop and often best managed with gentle packing of hemostatic materials rather than aggressive exploration
Medical management of elevated intracrainial pressure and the underlying brain injury is an essential part of patient care • Outcomes are often poor with mortality of 50%-90%. Survivors often have significant disabilities • In elderly the subdural hematoma can present several months after injury due to the space caused by brain atrophy and they are labeled as chronic subdural hematoma and outcomes post surgery are much better than acute subdural hematoma
Usually produce a focal injury pattern specific to the site of penetration • Gunshot wound that pass through the ventricular system are most often fatal • Management of less severe penetrating injury revolves around manging the potential infection ,complication of injury and repairing the breach of the skull Penetrating brain injury
Concussion • Is an immediate and transient loss of consciousness or normal mentation after head trauma often associated with period of amnesia • The severity of concussion appears to be proportional to the duration of amnesia particularly the anterograde amnesia • Who gets CT ? Diffuse brain injury diagnosis not typically requiring immediate surgical management
Validated clinical decision rules stress that all patient presenting with GSC of less than 15 , those that are vomiting , and those older than 60 to 65 are at high enough risk to warrant CT scan • Other factors warranting CT scan are sever headache, intoxication , persistent anterograde amnesia , a seizure with the injury , evidence of trauma to bone or soft tissue above the clavicle and severe mechanism of injury such as ejection injury
Management for isolated concussion in the ER includes a period of observation for at least 2 hours • Long term outcome are generally good however 25% of patients report an increased incidence of headache and memory difficulties even several months later • post concussive syndrome include depression, anxiety, memory loss , headache , emotional lability , insomnia • Treatment is reassurance
is bleeding into the subarachnoid space—the area between the arachnoid membrane and the pia mater surrounding the brain • Trauma is most common fallowed by cerebral aneurism Subarchnoidhemorrage
Occurs when the axons become sheared off between the boundary between gray and white matter during rapid brain acceleration or deceleration • Management is primarily medical Diffuse axonal injury
Seizure management • Homeostasis • Management of increased intracranial pressure by (venous drainage , CSF drainage, sedation, osmotic agent and diuretics, hyperventilation ,barbiturate, hypothermia , surgical decompression Medical management after traumatic brain injury
- More by User

HEAD INJURY. Mechanism of injury is generally a blow to the headVaries in presentation from concussion through loss of consciousness to coma and deathPrimarily MCA, MBA, pedestrians, falls from a height and sport. . HEAD INJURY PRIMARY LESIONS. Diffuse Axonal Injury (DAI)Contrecoup lesionsIntracranial/ Intracerebral Haemorraghes.
1.88k views • 25 slides

Head Injury
Head Injury. Anthony G. Hillier, D.O. St. John West Shore Emergency Medicine Resident. Head Injury-Epidemiology. 1.5 million Non-fatal TBI’s 370,000 Hospitalizations 80,000 cases of neurological sequela 52,000 Die from TBI’s 4 billion annually for cost of treatment Peak incidence:
1.28k views • 45 slides

Head Injury. Head Injury. Any trauma to the scalp , skull , or brain Head trauma includes an alteration in consciousness no matter how brief. Head Injury. Causes Motor vehicle accidents Firearm-related injuries Falls Assaults Sports-related injuries Recreational accidents. Head Injury.
2.45k views • 31 slides

Head Injury. LAMRT Nov 08. Head injuries. Pathophysiology of brain injury One million patients attend A+E each year in UK with head injury 80% are minor (GCS 13-15) 10% are moderate (GCS 9-12) 10% are severe (GCS <8) Severe head injuries account for 50% of trauma related deaths .
285 views • 7 slides

Head Injury. Presenters: Abraham Mani Moderator: Prof. D K Pawar. www.anaesthesia.co.in [email protected]. Classification of head injury. Mechanism of injury Outcome of the injury. Mechanism of injury . Non- missile or closed head injury . Acceleration – decelaration
3.27k views • 44 slides

Head Injury. Dr Malith Kumarasinghe MBBS (Colombo). Head Injuries:. Account for about one half of all trauma deaths Survivors range from baseline function to severe morbidity Even “minor” head injury can have severe impact As with most trauma, broken down into blunt and penetrating.
1.31k views • 62 slides

HEAD INJURY
HEAD INJURY . Augustine A. Adeolu Senior Lecturer and Consultant Neurosurgeon, COMUI, Ibadan NMA meeting, Oyo State , May. 2013. Objectives. Understanding of basic classification of head injuries Familiar with various causes of secondary brain assault/injury
927 views • 29 slides

Management of head injury . epidemiology. Head injury is a leading cause of morbidity and mortality and it is the most common cause of death among all patient suffering of traumatic injury. Motor vehicle accident are the most frequent cause of traumatic brain injury peaking in 15-24
1.09k views • 46 slides

An Overview of Head Injury Management
An Overview of Head Injury Management. Eldad J. Hadar, M.D. Department of Neurosurgery. Checklist. Definitions Glasgow Coma Scale Intracranial Pressure Mechanisms of brain injury Evaluation of head injury Management of head injury Operative Nonoperative. Head Injury Guidelines.
756 views • 35 slides

Head Injury. Saurabh Sinha Department of Clinical Neurosciences Western General Hospital. Age Groups. Mechanisms of Injury. What now?. Resuscitation. A airway with cervical spine control B breathing C circulation. Traumatic Brain Injury. Immediate impact injury
1.07k views • 56 slides

Head injury
Head injury. FM Brett MD FRCPath. At the end of this lecture you should be able to: Know basic facts about the incidence of head injury Know the difference between focal and diffuse injury Know the difference between missile and non-missile head injury Be able to classify ICH
667 views • 40 slides

Head injury. Dr. B.Padmashini Department of Accident, Emergency & Critical Care Medicine. Vinayaka Mission Kirupananda Variyar Medical College & Hospital. Salem,Tamil Nadu. Head Injury.
1.29k views • 68 slides

Management of Head Injury and Increased ICP
Management of Head Injury and Increased ICP. Nicole Baier , MD. Objectives. Review the: Epidemiology of head injury Various intracranial lesions Pathophysiology of increased ICP Management of head injury. Epidemiology. 2 cases per 1000 children per year Mild TBI: 82%
767 views • 50 slides

HEAD INJURY. E Woo. Non-penetrating head injury. Most controversial issues. Are the deficits consistent with the injury? Malingering? Is there any pre-existing disease that may cause or contribute to his deficits? Should he be cared for at home? What is the remaining life expectancy?.
804 views • 52 slides

Head injury. Presented by: Remya Gopinath. DEMOGRAPHIC DATA. Name: Case No.4 MR No : 185840 Diagnosis : RTA WITH HEAD INJURY Age: 6 YRS Gender: Male Date of admission: 2/10/2012.
3.5k views • 53 slides
Head Injury. Head Injury. A head injury is any trauma that leads to injury of the scalp, skull, or brain. The injuries can range from a minor bump on the skull to serious brain injury.
649 views • 33 slides

Head injury. FM Brett MD FRCPath. Head Injury - Facts Whether accidental, criminal or suicidal leading cause of death < 45 Accounts 1% of all deaths, 30% traumatic deaths and 50% of RTA deaths Severity assessed by GCS. GCS 1. Best eye response - (max 4)
1.54k views • 40 slides

Management of head injury. epidemiology. Head injury is a leading cause of morbidity and mortality and it is the most common cause of death among all patient suffering of traumatic injury. Motor vehicle accident are the most frequent cause of traumatic brain injury peaking in 15-24
2.02k views • 46 slides

Head injury triage, assessment, investigation and early management of head injury in infants, children and adults (update). Implementing NICE guidance. December 2007. NICE clinical guideline 56. Updated guidance.
566 views • 27 slides

Head Injury. Practical Aspects of Management and Transfer. Susanne Young. CONTENT. Head Injuries Background INITIAL MANAGEMENT Current Guidelines- ATLS Prevention of secondary Brain Injury (1-4) Use of adjunct therapies TRANSFER Which Sedative? AAGBI. BACKGROUND.
337 views • 12 slides

542 views • 31 slides

IMAGES
VIDEO
COMMENTS
This Google Slides and PPT template offers just that when it comes to delivering a presentation on head injuries. With a simple yet effective style and decorated with helpful illustrations, this template ensures a professional and engaging experience for both the presenter and viewers. What sets it apart is the AI-generated text that's included ...
Transcript. Slide 1-. 1 Management of the acute Head Injury Judith Fewings Consultant Therapist Neurosurgery. Slide 2-. 2. Slide 3-. OVERVIEW Traumatic brain injury (TBI) is a nondegenerative, noncongenital insult to the brain from an external mechanical force, with an associated diminished or altered state of consciousness.
Head Injury.ppt - Free download as Powerpoint Presentation (.ppt), PDF File (.pdf), Text File (.txt) or view presentation slides online. Scribd is the world's largest social reading and publishing site.
42 Thank you. Download ppt "Management of head injury". epidemiology Head injury is a leading cause of morbidity and mortality and it is the most common cause of death among all patient suffering of traumatic injury. Motor vehicle accident are the most frequent cause of traumatic brain injury peaking in Childe abuse is a common cause of head ...
Injuries to Head, Neck, and Face Concussions, neck sprains and strains, skull or neck fractures, facial lacerations, vision or hearing loss are only a few of the traumatic injuries that can affect the head, neck, and face. Coaches must be especially vigilant in managing these injuries if medical personnel is not present. Unfortunately, mismanagement can be the difference between complete ...
Slide 3-. Definition Head injury is defined as any trauma to the head other than superficial injuries to the face (NICE 2017) Traumatic brain injury (TBI) is a non specific term describing blunt, penetration or blast injuries to the brain. TBI can be classified as mild, moderate or severe, typically based on the GCS. Slide 4-.
This trauma PowerPoint presentation covers head injuries. Topics include: Anatomy. Concussion. Compression. Skull fractures. First aid management of head injuries. AVPU and GCS.
Management of head injury. epidemiology. Head injury is a leading cause of morbidity and mortality and it is the most common cause of death among all patient suffering of traumatic injury. Motor vehicle accident are the most frequent cause of traumatic brain injury peaking in 15-24. Download Presentation. injury. brain injury. epidural hematoma.
Head Injury. LAMRT Nov 08. Head injuries. Pathophysiology of brain injury One million patients attend A+E each year in UK with head injury 80% are minor (GCS 13-15) 10% are moderate (GCS 9-12) 10% are severe (GCS <8) Severe head injuries account for 50% of trauma related deaths . 284 views • 7 slides
An Image/Link below is provided (as is) to download presentation Download Policy: ... HEAD INJURIES. 704 views • 44 slides. Head, Neck, and Spine Injuries. Head, Neck, and Spine Injuries. Identify the most common causes of head, neck and spinal injuries. List 10 situations that might indicate serious head, neck and spinal injuries.
Features of the template. 100% customizable slides and easy to download. Slides are available in different nodes & colors. The slides contain 16:9 and 4:3 formats. Easy to change the colors quickly. It is a well-crafted template with an instant download facility. It is a 100% pre-designed slide. The slide holds vibrant icons.
Presentation Transcript. Management of head injury By : waleedalhoshan salehaljabri waelalmajed. Head injury is a leading cause of morbidity and mortality and it is the most common cause of death among all patient suffering of traumatic injury. Motor vehicle accident are the most frequent cause of traumatic brain injury peaking in 15-24 Childe ...